Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
Skin cancer screening is a vital proactive health practice designed to detect early-stage changes in the skin before they progress into more serious conditions. Because skin cancer is one of the most common malignancies in Singapore, regular clinical surveillance is essential—particularly for individuals with a history of significant sun exposure, those with a high number of moles, or those with a family history of skin cancer. While skin checks are often associated with identifying existing issues, a professional screening is primarily a preventative measure that provides peace of mind and identifies high-risk lesions at their most treatable stage.
Although skin cancer is a serious health concern, it is highly manageable when identified early. Success in skin health maintenance relies on three core pillars: regular self-monitoring for changes in skin lesions, professional dermatological assessment using dermoscopy to view beneath the skin's surface, and personalised, long-term surveillance schedules calibrated to your individual risk profile.



What Are Skin Cancers?
Skin cancers are abnormal growths that develop when DNA damage in skin cells—often triggered by UV radiation—leads to uncontrolled cell division. Unlike benign growths, which remain localised, some skin cancers have the potential to invade surrounding tissues or spread (metastasise) to other parts of the body.
The most common types are basal cell carcinoma, squamous cell carcinoma, and melanoma. Because early-stage skin cancers can mimic the appearance of harmless spots or moles, specialised dermatological care is required for accurate assessment and timely management.
What Are Common Types of Skin Cancer?
Accurate diagnosis is vital, as different types of skin cancer vary in their growth patterns and potential risks.
Basal Cell Carcinoma (BCC)
- Accounts for 70-80% of all skin cancers.
- Presents as skin-coloured or slightly reddish, pearly-looking bumps or chronic ulcers.
- Generally slow-growing, though they may bleed easily with minor trauma.
- Rarely metastasise, but require treatment to prevent local tissue destruction.
Squamous Cell Carcinoma (SCC)
- Makes up around 20% of skin cancers.
- Usually appears as reddish, rough, scaly bumps, often on chronically sun-exposed skin like the scalp, face, or back of the hands.
- Can occasionally break down to form an ulcer and has a higher risk of spreading to lymph nodes compared to BCC.
Malignant Melanoma
- A less common but highly aggressive form of skin cancer arising from melanocytes (pigment cells).
- Often mimics the appearance of normal moles, making professional dermoscopy essential for accurate diagnosis.
- Requires early detection and treatment to prevent spread to lymph nodes or other organs.
Actinic Keratosis (Pre-cancerous)
- Often described as pre-cancerous patches of dry, rough skin.
- Commonly found on the scalp, face, or hands of individuals with a history of long-term sun exposure.
- Essential to treat to prevent potential progression into squamous cell carcinoma.
Common Symptoms of Skin Cancer to Look Out For
Skin cancers often demonstrate progressive or distinct warning signs. Recognising these features early is the most effective way to ensure successful treatment. Monitor your skin for these signs:
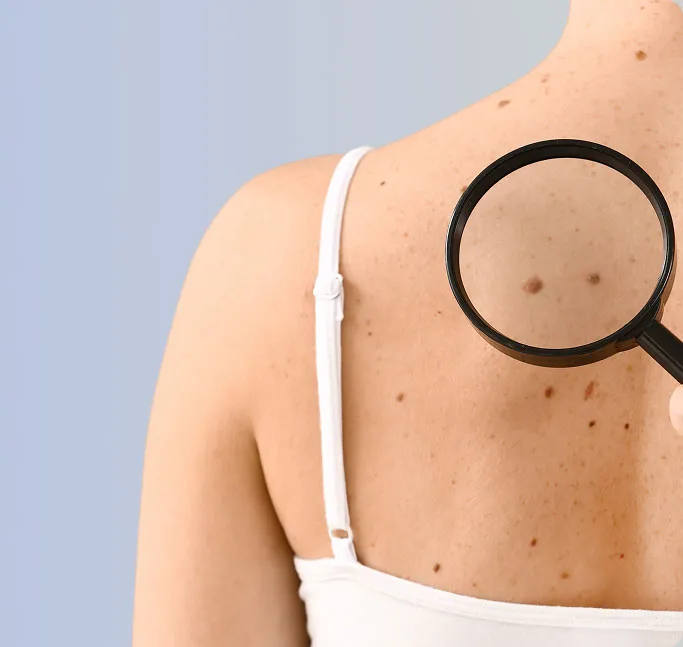
Changes in Appearance (The ABCDE Rules)
Persistent Non-Healing Sores
Unusual Surface Textures
Physical Sensations
Spontaneous Bleeding or Crusting
The Ugly Duckling Sign
What Causes or Triggers Skin Cancer?
Skin cancer arises when genetic mutations occur within skin cells, causing them to grow uncontrollably and form malignant lesions. While some factors are beyond our control, understanding these triggers is essential for effective prevention and early detection.
Cumulative Sun Exposure
Genetic Predisposition
Weakened Immune System
History of Pre-cancerous Lesions
Chronic Inflammation or Scarring
Chemical and Environmental Exposure
How Are Skin Cancers Diagnosed?
Accurate diagnosis is the cornerstone of effective skin cancer management. Because skin cancers often masquerade as harmless spots or benign growths, a structured, professional evaluation is essential to identify malignancy at the earliest possible stage.
Clinical Examination
Medical History Review
Advanced Dermoscopy
Skin Biopsy
How Are Skin Cancers Screened at TSN Dermatology?
A skin cancer screen or mole check is a thorough skin examination by a specialist. This can sometimes take more than 30 minutes. A dermatologist will usually use a dermatoscope, a specialised tool that helps to identify unique patterns under the skin, to help make a more accurate diagnosis.
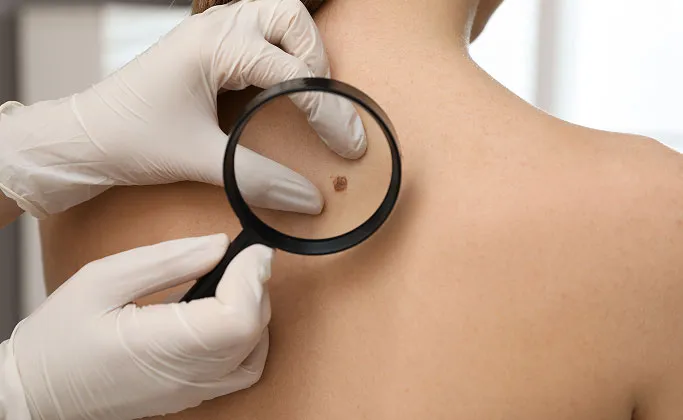
At TSN Dermatology, evaluation usually begins with a comprehensive medical history assessment to identify the risk level a patient has for skin cancer. This is followed by examination, firstly of the growths that the patient is worried about, and then the rest of the skin from head to toe. We aim to be thorough, but will protect your modesty and make you comfortable at all times.
If any suspicious growth is identified, our doctor will discuss with you the options available, ranging from close observation of the growth to taking a skin biopsy. The consultation ends with education on how to perform self-monitoring of the skin and sun protection. Regular skin checks by the doctor should be performed every 6 to 12 months.
Tips on Daily Care and Prevention of Skin Cancer
While skin cancer is often driven by genetics and past cumulative UV damage, consistent daily habits are your most powerful tool for prevention and early detection. Whether you are proactively protecting your skin or recovering from a recent treatment, these habits are essential for long-term health.
Sun Safety: Your First Line of Defence
-
Use Broad-Spectrum Sunscreen
Apply a high-SPF (30 or higher), broad-spectrum sunscreen daily to all exposed skin, regardless of the weather. Reapply every two hours if you are outdoors. -
Practice Sun-Smart Living
In Singapore's intense tropical climate, minimise direct sun exposure between 10 AM and 4 PM. Use protective gear like wide-brimmed hats, UV-blocking sunglasses, and long-sleeved, breathable clothing to create a physical barrier against harmful radiation. -
Seek Shade
Whenever possible, stay under cover. Remember that reflective surfaces like sand, water, and concrete can increase your UV exposure even when you are not in direct sunlight.
Perform Monthly Self-Exams
-
The ABCDE & Ugly Duckling Check
Spend 5-10 minutes once a month examining your skin. Use a full-length mirror and a hand mirror to check areas you cannot easily see, such as your back, scalp, soles of your feet, and between your toes. -
Know Your Baseline
Familiarise yourself with your existing moles. The goal of these self-exams is to identify the Ugly Duckling—any spot that looks, feels, or behaves differently than your other moles, or a spot that is evolving in size, shape, or colour.
Maintain Skin Health and Immunity
-
Be Mindful of Lifestyle Factors
While UV is the primary trigger, maintaining a healthy, balanced lifestyle supports your immune system—your body's internal defence against abnormal cell growth. -
Monitor High-Risk Areas
If you have a history of chronic inflammation, long-standing ulcers, or burn scars, keep a close watch on these areas. Skin cancer can occasionally develop in tissues that have been chronically damaged or scarred.
Post-Treatment Aftercare
-
Strict Wound Care
If you have undergone a procedure (such as excision or Mohs surgery), strictly follow your dermatologist's wound care instructions to prevent infection and promote optimal healing. -
Protect the Healing Site
The skin at a surgical site is fragile. Keep it protected from the sun with clothing or high-SPF sunscreen to prevent permanent hyperpigmentation and ensure the best cosmetic outcome. -
Attend All Follow-up Appointments
Regular surveillance is critical for patients with a history of skin cancer. Even if an area looks fully healed, these check-ups ensure that no recurrent or new lesions are missed.



When Should You See a Dermatologist for Skin Cancer Screening?
Early detection is the most significant factor in successfully treating skin cancer. Because many malignancies can deceptively mimic harmless moles or benign spots, you should not rely on a wait-and-see approach if you have concerns. You should schedule a professional skin cancer screening or a dedicated mole check if you experience any of the following:
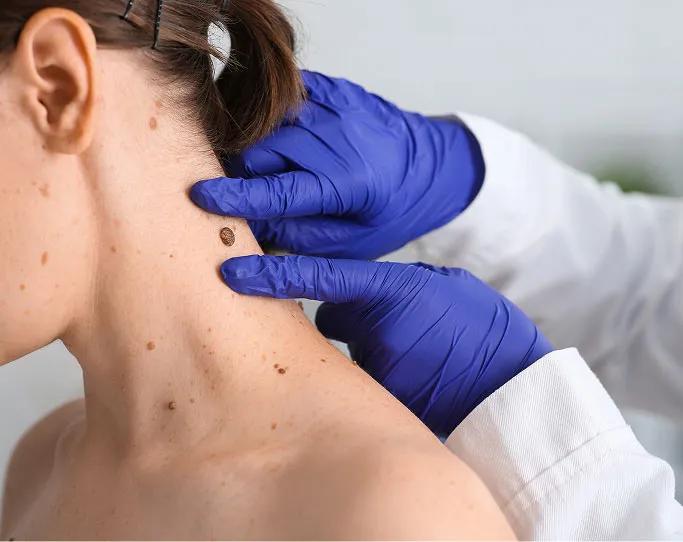
New or Evolving Spots
Any new mole appearing after age 30, or any existing spot that is visibly changing in size, shape, symmetry, or colour, requires immediate evaluation.
Non-Healing Sores
If you have a sore, ulcer, or crusted patch that fails to heal after several weeks—or one that heals and then repeatedly returns in the same spot—it must be assessed to rule out basal cell or squamous cell carcinoma.
The Ugly Duckling Sign
If you notice a spot that looks significantly different, darker, or more irregular compared to the rest of your moles, it stands out as a potential red flag and should be examined.
Persistent Symptoms
A growth that becomes persistently itchy, tender, or painful, or one that bleeds or weeps without any clear history of injury, requires urgent clinical investigation.
Risk Factor History
If you have a personal or family history of skin cancer (especially melanoma), a history of severe blistering sunburns, or a fair complexion, you should undergo regular, proactive skin checks even if you don't notice any specific changes.
Total Body Surveillance
If you have an extensive number of moles, it can be difficult to track changes at home. A professional skin check every 6 to 12 months provides a baseline and the expert oversight needed to detect subtle, dangerous changes that may be missed during self-examination.
FAQs About Skin Cancer Screening
No. Skin cancer is not contagious and cannot be spread through physical contact, sharing personal items, or social interaction. It is the result of uncontrolled cell growth caused by internal genetic mutations, typically triggered by external factors like cumulative UV radiation.
Yes, especially when detected early. For the vast majority of skin cancers, complete surgical removal—often requiring only minor, localised excision—is curative. For advanced cases, modern therapies like immunotherapy or targeted treatments can also achieve excellent control. Because skin cancer is often a marker of cumulative sun damage, however, patients remain at a higher risk of developing new lesions elsewhere, which is why regular long-term surveillance is crucial.
It is often a combination of your genetic blueprint and your unique history of sun exposure. Factors like skin type (fairer skin provides less natural protection), the amount of time spent outdoors, a history of blistering sunburns, and the efficiency of your immune system all play a role in whether your cells successfully repair UV-induced damage or develop into cancer.
No. Unlike some rare inflammatory skin conditions, skin cancers do not regress or disappear on their own. While a lesion might occasionally scab over or seem to shrink temporarily, this is often a deceptive sign of healing that masks underlying tumour growth. Any lesion that changes or fails to heal must be evaluated by a professional.
Seek Proper Dermatologist Care for Skin Cancer
If you suspect you or your child might have skin cancer, a consultation with our specialists at TSN Dermatology Skin Specialist Clinic can help clarify the diagnosis and establish an effective, personalised treatment plan focused on long-term skin health and quality of life. For more information or appointments, please contact us today.
Meet TheDoctors Behind Your Care

Dr Koh Hong Yi
Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in Skin Cancer Screening, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh