Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
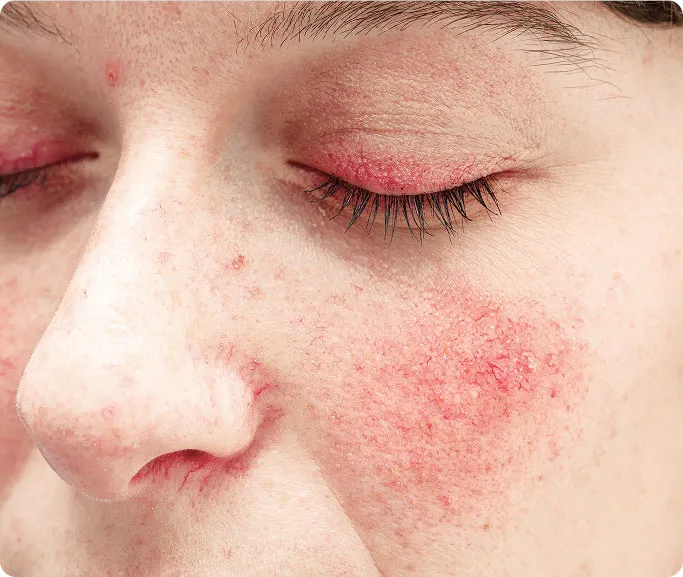
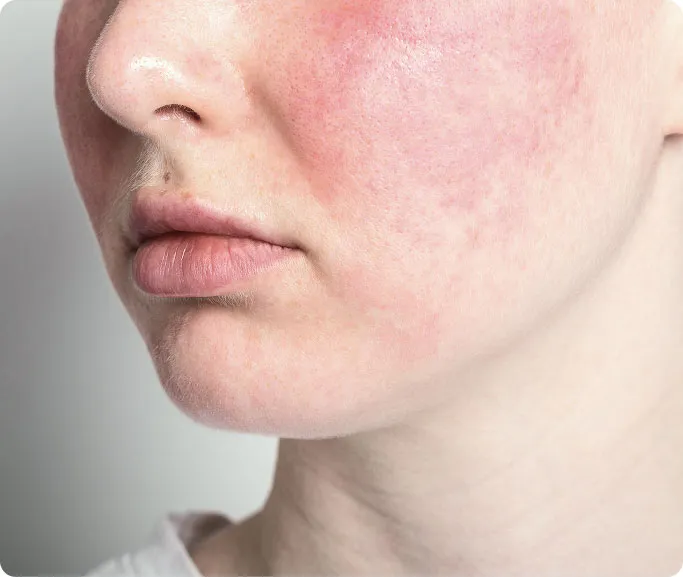
Rosacea is a common, chronic inflammatory skin condition that primarily affects the central face, including the cheeks, nose, chin, and forehead. It typically manifests as persistent redness (erythema), visible broken blood vessels (telangiectasia), and sometimes acne-like bumps or pustules.
While commonly diagnosed in individuals between the ages of 30 and 50, rosacea can occur at any age. While there is no permanent cure, modern dermatological treatments can effectively manage redness, prevent progression, and significantly improve skin comfort and appearance.




What Is Rosacea?
Rosacea is a chronic skin condition that causes persistent facial redness, flushing, and sometimes acne-like bumps. It occurs when the skin becomes overly sensitive and prone to inflammation, often involving increased activity of the blood vessels in the face. Common triggers include:
Environmental Factors
Exposure to UV sunlight, extreme heat or cold, and strong winds.
Lifestyle Triggers
Consumption of spicy foods, hot beverages, or alcohol, which can induce vasodilation.
Emotional Stress
Significant stress can trigger flare-ups in many patients.
Topical Irritants
Certain skincare products or harsh cleansers can disrupt the skin barrier, increasing sensitivity.
Because rosacea is a chronic condition that can worsen if left unmanaged, it requires professional dermatological assessment to identify your specific triggers, manage vascular inflammation, and protect the skin barrier to prevent long-term redness and structural changes.
What Are Common Types of Rosacea?
Rosacea does not look the same for everyone and can present with different symptoms, such as persistent redness, acne-like bumps, or thickened skin. Identifying the type of rosacea helps guide the most effective treatment approach.
Erythematotelangiectatic Rosacea (ETR)
Ocular Rosacea
Papulopustular Rosacea
Neurogenic Rosacea (Sensory)
Phymatous Rosacea
Persistent Edema
Common Symptoms of Rosacea to Look Out For
Rosacea symptoms can be highly variable and often progress through different stages. While it is primarily a condition of facial blood vessels and inflammation, symptoms can extend to the eyes and skin texture. The following are the most common signs to monitor:

Persistent Facial Redness (Erythema)
Often the earliest sign, this is a persistent redness in the central part of your face (the sun-kissed area: cheeks, nose, forehead, and chin). It can look like a mild sunburn that never fades.
Visible Broken Blood Vessels (Telangiectasia)
As the condition progresses, small, thread-like blood vessels become visible beneath the surface of the skin, particularly on the cheeks and around the nose.
Papules and Pustules
Many people with rosacea develop small, red, solid bumps (papules) or pus-filled pimples (pustules) that resemble teenage acne. However, unlike acne, these lesions are not associated with oily skin and are typically tender or stinging.
Ocular Symptoms
Many patients experience eye-related symptoms, often referred to as ocular rosacea. This includes eyes that appear watery or bloodshot, a persistent dry or gritty sensation, burning, stinging, or increased light sensitivity.
Skin Thickening and Texture Changes
In advanced cases, the skin can thicken and develop a bumpy, irregular texture. When this occurs on the nose, it is known as rhinophyma, leading to an enlarged, bulbous, and reddish appearance. This is significantly more common in men than in women.
Stinging and Burning Sensations
The skin affected by rosacea is often hypersensitive. Patients frequently report a burning or stinging sensation, even when using gentle skincare products or when exposed to mild environmental changes like wind or air conditioning.
Swelling (Edema)
Chronic inflammation can lead to fluid retention in the facial tissues. You may notice swelling, particularly around the eyes or on the cheeks, which can feel tight and contribute to a feeling of facial discomfort.
What Causes or Triggers Rosacea?
Rosacea is influenced by a combination of genetic and environmental factors. Many people experience flare-ups when certain triggers cause the blood vessels in the face to dilate, leading to redness and inflammation.
Genetic Predisposition and Immune Response
Neurovascular Dysregulation
Environmental Triggers
Environmental factors are a common cause of rosacea flare-ups.
-
Sun Exposure
UV radiation is one of the most common triggers and can worsen redness and sensitivity. -
Temperature Extremes
Heat, cold weather, or strong winds can trigger flushing. -
Humidity and Sweat
High humidity and sweating may irritate the skin and worsen inflammation.
Lifestyle and Dietary Triggers
Certain lifestyle choices are well-documented to induce vasodilation (widening of blood vessels):
-
Dietary Irritants
Spicy foods, hot beverages, and alcohol are common triggers. -
Emotional Stress
High-stress environments trigger the body's fight or flight response, which can cause sudden, intense facial flushing.
Topical Irritants and Skin Barrier Damage
Medications
How Is Rosacea Diagnosed?
Diagnosing rosacea is done through an evaluation of your history, symptoms, and the patterns of your skin changes. A dermatologist's goal is to identify your subtype and rule out other conditions that cause facial redness.
Clinical Examination
Medical History Review
Eye Examination
Excluding Similar Conditions
Skin Biopsy (When Necessary)
How Is Rosacea Treated at TSN Dermatology?
At TSN Dermatology, rosacea treatment is tailored to each patient's symptoms and triggers. Management may include topical medications, oral treatments, and lifestyle adjustments to reduce redness, control inflammation, and prevent flare-ups.

Topical Therapies
Topical medications are commonly used to manage redness, inflammation, and acne-like bumps associated with rosacea. These treatments are applied directly to the skin to help calm irritation and reduce visible symptoms.
Anti-Inflammatory Creams
Prescription topical medications help reduce inflammation and control papules and pustules, improving the appearance of rosacea-prone skin.
Vasoconstrictor Agents
Certain topical treatments temporarily constrict dilated blood vessels in the skin, helping reduce persistent facial redness.
Laser and Light Therapy (Vascular Targeted)
For patients with visible blood vessels or persistent background redness, laser and light-based treatments can help target the underlying vascular changes in rosacea.
Vascular Lasers (e.g., Pulsed-Dye Laser)
These lasers target the hemoglobin in dilated blood vessels, helping reduce visible thread-like vessels and long-standing facial redness.
Intense Pulsed Light (IPL)
IPL uses controlled light energy to reduce diffuse redness and improve overall skin tone by targeting superficial blood vessels.
Systemic Therapies
When rosacea is more severe or does not respond well to topical treatments alone, oral medications may be recommended to control inflammation.
Oral Anti-Inflammatory Medications
Low-dose oral treatments help reduce inflammation throughout the skin and control persistent bumps and breakouts associated with rosacea.
Ocular and Advanced Care
Rosacea can sometimes affect the eyes or cause thickening of facial skin. In these cases, specialised management may be required.
Ocular Rosacea Management
If rosacea affects the eyes, treatment may include eyelid hygiene, lubricating eye drops, or anti-inflammatory medications to protect eye health.
Management of Rhinophyma
For phymatous rosacea, where the skin becomes thickened (commonly on the nose), dermatological procedures may be used to improve skin texture and contour.
Tips on Daily Care and Prevention for Rosacea
For individuals living with rosacea, daily care focuses on calming the skin, protecting the skin barrier, and identifying triggers that cause flushing or irritation. Gentle skincare and avoiding common triggers can help reduce flare-ups and keep symptoms under better control.
Gentle Skin Handling and Protection
-
Use Gentle, Non-Irritating Skincare
Avoid harsh cleansers, toners with alcohol, mechanical scrubs, or products containing fragrance, menthol, or witch hazel. -
Sun Protection is Important
UV radiation is a common trigger for rosacea. Use a mineral-based sunscreen as these are generally less irritating to sensitive skin. -
Pat, Never Rub
When cleansing or applying products, use a gentle patting motion. Rubbing and tugging on the skin creates friction, which can stimulate blood flow and trigger a flush.
Trigger Identification and Management
-
Maintain a Trigger Diary
Track your daily activities, food intake, and environmental exposures alongside your skin's reaction. -
Manage Thermal Stress
Since heat is a vascular trigger, try to stay in cool environments. If you are exercising, keep a cool, damp cloth nearby to gently dab on your face if you start to feel overheated. -
Minimize Emotional Stress
High stress can lead to sudden flushing. Incorporate mindfulness or relaxation practices to manage the physiological stress response.
Itch and Stinging Control
-
Cool Compresses
If your face feels hot or is stinging, a cool compress can help constrict blood vessels and soothe the inflammation. -
Keep it Simple
When your skin is flaring, simplify your routine. Stick to the essentials like a gentle cleanser, a soothing moisturizer, and your sunscreen.
Environmental and Lifestyle Factors
-
Watch the Wind and Cold
Cold air, strong winds, and rapid temperature changes can trigger a flush. -
Dietary Adjustments
Some people find relief by limiting very hot beverages, spicy meals, and alcohol. Test these individually to see what affects your skin.
Proactive Care and Early Intervention
-
Be Proactive
If you notice your skin is becoming constantly red or you see new small, broken blood vessels appearing, seek medical care from a dermatologist. -
Medications
Use your prescribed creams as directed. Sometimes, your dermatologist may advise continuing certain treatments to maintain the vascular stability of your face.



When Should You See a Dermatologist for Rosacea?
While mild rosacea symptoms may sometimes be managed with gentle skincare and trigger avoidance, medical treatment may be needed when symptoms become persistent or more severe. You should consider seeing a dermatologist if you experience the following:

Persistent Redness
If your facial flushing does not subside or if you notice permanent, background redness that looks like a lasting sunburn, this indicates chronic vascular inflammation that requires medical suppression.
Visible Broken Blood Vessels
If you notice small, thread-like vessels (telangiectasia) appearing on your cheeks or nose, these are permanent changes that generally require more advanced laser or light-based treatments to fade.
Acne-Like Bumps and Pustules
If you develop persistent red bumps or pus-filled pimples that do not respond to standard acne treatments, you likely have papulopustular rosacea, which requires prescription-strength anti-inflammatory topicals.
Eye Irritation
If your eyes feel persistently gritty, dry, or sandy, or if you have red, bloodshot eyes or light sensitivity, you may have ocular rosacea. This requires a professional assessment to prevent potential complications affecting your vision.
Skin Thickening or Swelling
If you notice the skin on your nose or cheeks becoming bumpy, irregular, or bulbous (rhinophyma), seek help immediately. Early intervention is critical to stop and reverse these structural changes.
Significant Social Impact
If the redness or the physical sensation of burning and stinging is affecting your quality of life, confidence, or daily activities, modern treatments can significantly reduce your symptoms and soothe your skin.
FAQs About Rosacea
No. Rosacea is not an infection and cannot be spread through physical contact, sharing personal items, or any form of interaction. It is a chronic inflammatory and vascular condition of the skin.
Rosacea is not directly inherited, but genetics may play a role. People with a family history of rosacea may have a higher likelihood of developing the condition, although it does not occur in every case.
Rosacea is a chronic condition, so there is currently no permanent cure. However, with appropriate treatment and trigger management, most people can effectively control symptoms and reduce flare-ups.
Frequent flushing is a common symptom of rosacea. It happens because the blood vessels in the face are more sensitive and easily widen in response to triggers such as heat, spicy foods, alcohol, exercise, or stress. Identifying and avoiding your personal triggers can help reduce flare-ups.
Diet can affect rosacea in some people. Certain foods and drinks—such as spicy foods, hot beverages, alcohol, and foods high in histamines—may trigger flushing or worsen symptoms. Identifying and limiting personal dietary triggers can help reduce flare-ups.
Skin thickening is a less common form of rosacea known as phymatous rosacea. It does not occur in most patients, but when it does, it typically develops gradually over time. Early diagnosis and treatment can help control rosacea and reduce the risk of skin thickening.
Seek Proper Dermatologist Care for Rosacea
If you or your child are experiencing Rosacea, a consultation with our specialists at TSN Dermatology Skin Specialist Clinic can help clarify the diagnosis and establish an effective, personalised treatment plan focused on long-term skin health and quality of life. For more information or appointments, please contact us today.
Meet TheDoctors Behind Your Care

Dr Koh Hong Yi
Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in rosacea treatment, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh