Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
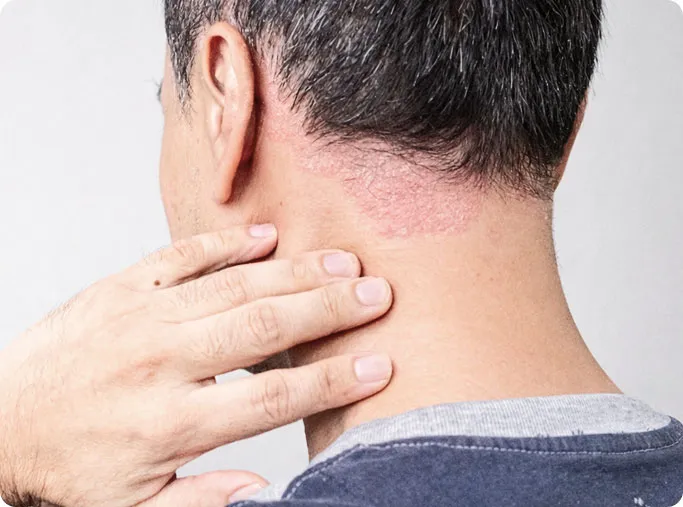
Psoriasis is a common, inflammatory skin condition that affects approximately 2-3% of the population worldwide. It manifests as a systemic immune-mediated response that accelerates the skin's growth cycle, resulting in red, thick, and flaky patches (plaques). While these plaques most commonly appear on the scalp, elbows, knees, lower back, and buttocks, the condition can also impact the nails, causing them to become misshapen, pitted, or discolored.
In some cases, the condition extends beyond the skin - some patients may develop psoriatic arthritis (PsA), which leads to chronic joint pain, swelling, and potential deformity. While many individuals develop psoriasis in their 20s or 50s, it can occur at any age. Although psoriasis is a chronic condition, modern dermatological therapies can significantly reduce inflammation, clear the skin, and improve overall quality of life.



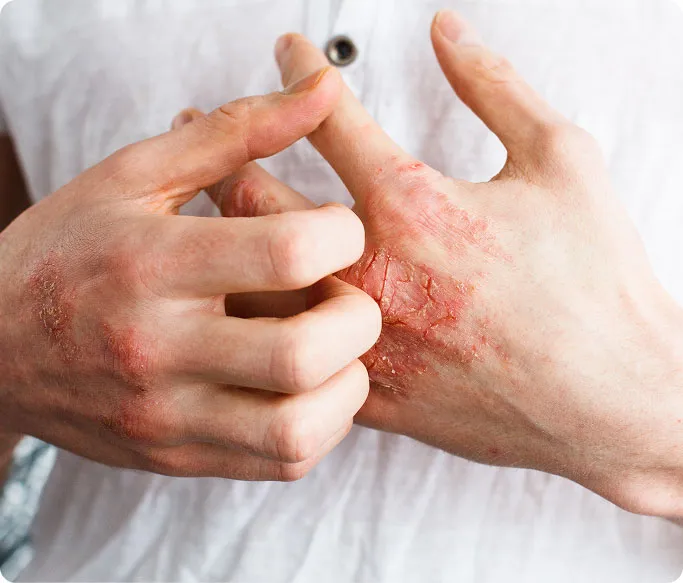
What Is Psoriasis?
Psoriasis is the result of an overactive immune system within the skin. Normally, skin cells grow and shed over the course of weeks. In psoriasis, however, this process happens in a matter of days. This rapid turnover, combined with persistent inflammation, causes the skin to thicken and form the characteristic raised, scaly plaques.
Psoriasis is more than just dry skin. It is a complex immune-mediated disorder with a strong genetic component—more than 30 genes have been identified as being associated with its development. Environmental factors act as the spark, with triggers such as high stress, bacterial infections, certain medications, and physical trauma to the skin often inducing a flare-up. Because psoriasis can involve systemic health, including the joints and nails, it requires professional dermatological management to control inflammation and prevent long-term complications.
What Are Common Types of Psoriasis?
Psoriasis is a highly variable condition. Dermatologists classify it based on the appearance of the lesions, the body sites involved, and the specific systemic impact. Understanding your specific classification is key to selecting the most effective treatment.
Plaque Psoriasis (Psoriasis Vulgaris)
Guttate Psoriasis
Scalp Psoriasis
Inverse Psoriasis
Pustular Psoriasis
Erythrodermic Psoriasis
Psoriatic Arthritis
Nail Psoriasis
Common Symptoms of Psoriasis to Look Out For
Psoriasis symptoms can vary depending on the type and severity of the condition. While the classic presentation involves raised, scaly patches on the skin, some people may also experience changes affecting the nails, joints, or other parts of the body. The following are some common signs to watch for:
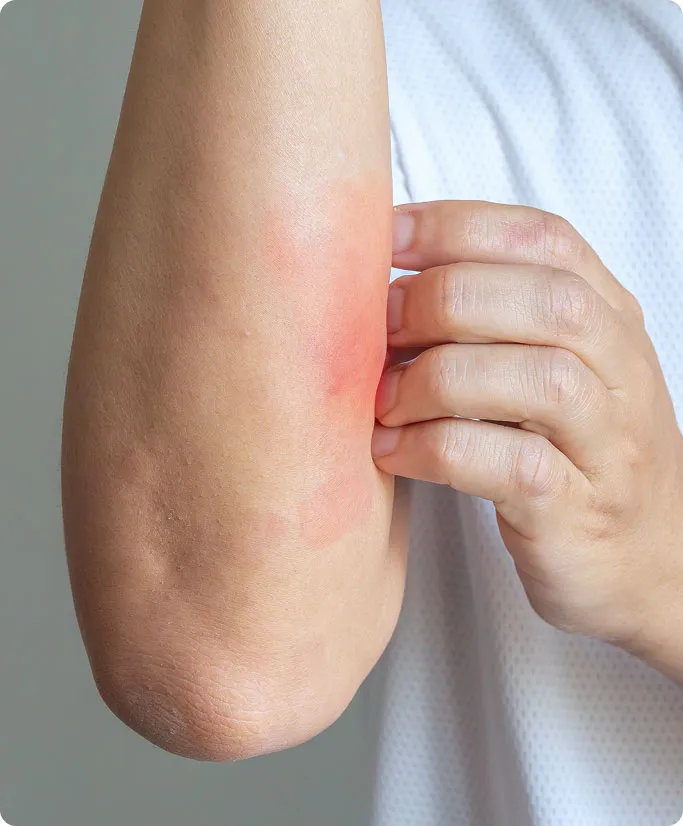
Raised, Red, and Inflamed Plaques
The hallmark of plaque psoriasis is the development of raised, red skin lesions. These patches are often well-defined, meaning they have a distinct border separating the inflamed skin from healthy, surrounding skin.
Silvery-White Scales
Most psoriasis plaques are topped with a thick, silvery-white buildup of dead skin cells. This scale is often dry and can shed or flake away, revealing red, shiny skin underneath that may bleed slightly if the scale is picked or scratched.
Intense Itching and Burning
While psoriasis is often described as itchy, the sensation can range from mild annoyance to an intense, burning, or stinging sensation. The itch is usually localized to the plaques and can become significantly more uncomfortable during a flare-up.
Nail Changes
Psoriasis frequently affects the nails. Common symptoms include nail pitting (small, pin-prick dents in the nail surface), thickening of the nail plate, discoloration (often described as oil drop spots beneath the nail), or onycholysis (the nail lifting away from the nail bed).
Skin Fissures and Cracking
In areas of thick skin or where plaques cover joints (such as the elbows or knees), the skin may become so dry and tight that it develops deep, painful fissures or cracks. These can bleed and are often highly susceptible to secondary bacterial infections.
Joint Pain and Swelling
For patients who develop psoriatic arthritis, symptoms include persistent joint pain, stiffness (particularly in the morning), and localized swelling. You may notice sausage-like swelling of the fingers or toes, or pain in the lower back or heels.
Scalp Crusts and Flaking
Psoriasis on the scalp often presents as thick, crusted plaques that can be mistaken for severe dandruff. Unlike simple dandruff, these plaques are often firmly attached to the scalp and can extend beyond the hairline onto the forehead, ears, or neck.
Smooth Lesions in Folds (Inverse Psoriasis)
When psoriasis occurs in body folds—such as the armpits or groin—it typically lacks the classic silvery scale due to friction and moisture. Instead, the area appears as a smooth, shiny, and bright red patch, which may be tender or prone to yeast infections.
What Causes or Triggers Psoriasis?
Psoriasis develops due to an overactive immune response that speeds up the skin cell growth cycle. While the exact cause is not fully understood, several factors are known to trigger the onset of psoriasis or worsen existing symptoms. They include:
Genetic Predisposition
Immune System Dysregulation
Emotional and Physiological Stress
Physical Trauma
Infections
Medications
Lifestyle and Environmental Factors
-
Smoking and Alcohol
Both are linked to increased frequency and severity of psoriasis flares. Smoking can also reduce the skin's ability to heal and respond effectively to treatment. -
Climate
In Singapore's hot, humid climate, sweat can be an irritant for inverse psoriasis (in skin folds), while cold, dry environments can often cause plaque psoriasis to dry out and crack.
How Is Psoriasis Diagnosed?
Psoriasis is usually diagnosed by a dermatologist through a physical examination of the skin. Since its symptoms can resemble other skin conditions such as eczema or fungal infections, careful evaluation is important.
Clinical Examination
Medical History Review
Physical Assessment of Nails and Joints
Skin Biopsy
Blood and Imaging Tests
Exclusion of Mimics
Psoriasis can look very similar to other conditions. Your dermatologist is trained to distinguish it from:
-
Eczema
Which often lacks the distinct silvery scale and affects different skin areas. -
Fungal Infections
Which can be ruled out through skin scrapings if there is doubt. -
Seborrheic Dermatitis
Particularly when scalp involvement is present.
How Is Psoriasis Treated at TSN Dermatology?
At TSN Dermatology, psoriasis treatment is tailored to each patient's condition and symptoms. Depending on the severity and extent of psoriasis, management may include topical medications, phototherapy, or systemic treatments to control inflammation and reduce flare-ups.
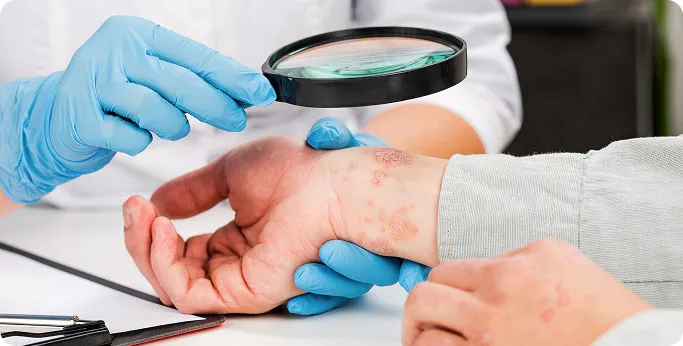
Individualised Treatment Approach
Our dermatologists assess the severity of the psoriasis, including the extent of skin involvement and the impact on daily life. Treatment considers the specific areas affected, such as the scalp, skin folds, or nails. Because psoriasis can sometimes be associated with joint inflammation or metabolic conditions, we also monitor for signs of psoriatic arthritis and other related health concerns. As psoriasis is a chronic condition, the goal is to achieve clear or well-controlled skin while maintaining long-term stability through regular follow-up care.
Topical Therapies
For mild to moderate psoriasis, topical medications are often the first line of treatment. These may include medicated creams, ointments, or lotions such as topical corticosteroids, vitamin D analogues, or calcineurin inhibitors to reduce inflammation and slow excessive skin cell growth. For scalp psoriasis, specialised foams, gels, or medicated shampoos may be used to help lift thick scales and deliver treatment directly to the affected areas.
Phototherapy (Light Therapy)
For patients with more widespread psoriasis or when topical treatments alone are insufficient, medical phototherapy may be recommended. Narrowband UVB therapy uses specific wavelengths of ultraviolet light to reduce inflammation and slow the rapid turnover of skin cells. This treatment is non-invasive and suitable for many patients under medical supervision.
Systemic and Biologic Therapies
For moderate to severe psoriasis, or when the condition affects larger areas of the body, systemic treatments may be considered. Oral medications can help control inflammation throughout the body, while biologic therapies target specific pathways in the immune system that drive psoriasis. These treatments are often highly effective in controlling persistent or severe disease.
Nail and Joint Involvement
Psoriasis can also affect the nails and joints. Nail psoriasis may cause pitting, thickening, or separation of the nail from the nail bed, which may require targeted treatments. If symptoms suggest possible psoriatic arthritis, early referral to a rheumatologist may be recommended to ensure timely management and protect long-term joint health.
Tips on Daily Care and Prevention for Psoriasis
For individuals living with psoriasis, daily care is focused on maintaining the skin's barrier, reducing inflammation, and preventing flare-ups triggered by environmental or physical stress. While psoriasis is a chronic condition, these consistent habits can help you achieve longer periods of remission and keep your skin comfortable.
Gentle Skin Handling and Moisturisation
-
Hydrate Frequently
Use thick, fragrance-free creams or ointments rather than thin lotions. Moisturising immediately after bathing helps lock in water. -
Gentle Cleansing
Avoid hot showers, which strip natural oils and worsen inflammation. Use lukewarm water and mild, soap-free, or lipid-replenishing cleansers. Pat your skin dry with a soft towel—never rub.
Trigger Identification and Management
-
Maintain a Trigger Diary
Track potential triggers like high stress, infections, specific foods, or changes in the weather. -
Manage Stress
Since stress is a common trigger, lowering your physiological stress levels helps calm the immune system's inflammatory response. -
Avoid Skin Trauma
Be careful to avoid cuts, scrapes, or severe sunburns, as physical injury to the skin can induce a new psoriasis plaque at the site of trauma.
Itch Control and Skin Comfort
-
Do Not Scratch
Scratching damages the skin, creates inflammation, and encourages the psoriasis to grow. -
Wear Breathable Fabrics
In Singapore's climate, sweat can irritate plaques, particularly in skin folds. Opt for loose-fitting, natural fibres like cotton or bamboo that allow your skin to breathe and minimize moisture buildup.
Proactive Health and Medication Adherence
-
Be Consistent with Treatments
Psoriasis treatments work best when used exactly as prescribed. -
Monitor Nails and Joints
Check your nails for pitting or thickening, and stay mindful of joint pain, stiffness, or swelling. Early detection of psoriatic arthritis allows for timely intervention to prevent joint damage. -
Avoid Known Triggers
If you are a smoker or consume alcohol regularly, consider reducing or eliminating these habits, as both are associated with more frequent and severe psoriasis flares.



When Should You See a Dermatologist for Psoriasis?
A dermatologist should evaluate psoriasis if symptoms are persistent, worsening, or not responding to basic treatments. Specialist care may also be needed when psoriasis affects sensitive areas such as the scalp, nails, or joints. You should seek medical attention if you experience the following:

Rapidly Spreading or Widespread Plaques
If psoriasis plaques appear suddenly across multiple body areas or begin covering larger portions of skin, medical treatment may be required to control the flare.
Joint Pain or Stiffness
Persistent joint pain, swelling, or morning stiffness may indicate psoriatic arthritis. Early evaluation is important to prevent long-term joint damage.
Nail Changes
Pitting, thickening, discoloration, or crumbling of the nails may indicate nail psoriasis, which often requires targeted medical treatment.
Symptoms Not Improving with Over-the-Counter Care
If moisturisers or non-prescription treatments do not improve redness, scaling, or itching after several weeks, prescription therapies may be needed.
Significant Impact on Daily Life
If psoriasis causes severe itching, sleep disturbance, emotional distress, or difficulty with daily activities, a dermatologist can recommend treatments to better control symptoms.
Signs of Infection or Painful Cracking
If plaques become moist, develop yellow crusting, or form deep painful cracks, medical attention is needed to treat possible infection.
Uncertain Diagnosis
If you have a persistent red, scaly rash and are unsure whether it is psoriasis or another condition such as eczema or a fungal infection, a dermatologist can confirm the diagnosis and guide appropriate treatment.
FAQs About Psoriasis
No. Psoriasis is an immune-mediated inflammatory condition, not an infection. It cannot be spread through physical contact, sharing personal items, or interacting with others.
Psoriasis is a chronic condition, which means there is currently no permanent cure. However, it is highly manageable with appropriate medical treatment. Many patients can achieve long periods where symptoms are well controlled or minimal with the right treatment plan and ongoing care.
No. Although psoriasis appears on the skin, it is an immune-related condition that can affect other parts of the body. In some patients, it may also involve the joints (psoriatic arthritis) or be associated with other health conditions like metabolic syndrome.
Certain foods may trigger or worsen psoriasis symptoms in some individuals, although triggers can vary from person to person. Commonly reported triggers include alcohol, highly processed foods, and foods high in sugar or saturated fats. Maintaining a balanced diet and identifying personal triggers may help reduce flare-ups.
Nail psoriasis can be persistent, but it is treatable. If left untreated, it may lead to lasting changes in the nails, such as thickening, pitting, or separation from the nail bed. Early treatment can help control symptoms and reduce the risk of permanent nail damage.
Seek Proper Dermatologist Care for Psoriasis
If you or your child are experiencing Psoriasis, a consultation with our specialists at TSN Dermatology Skin Specialist Clinic can help clarify the diagnosis and establish an effective, personalised treatment plan focused on long-term skin health and quality of life. For more information or appointments, please contact us today.
Meet TheDoctors Behind Your Care

Dr Koh Hong Yi
Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in psoriasis treatment, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh