Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
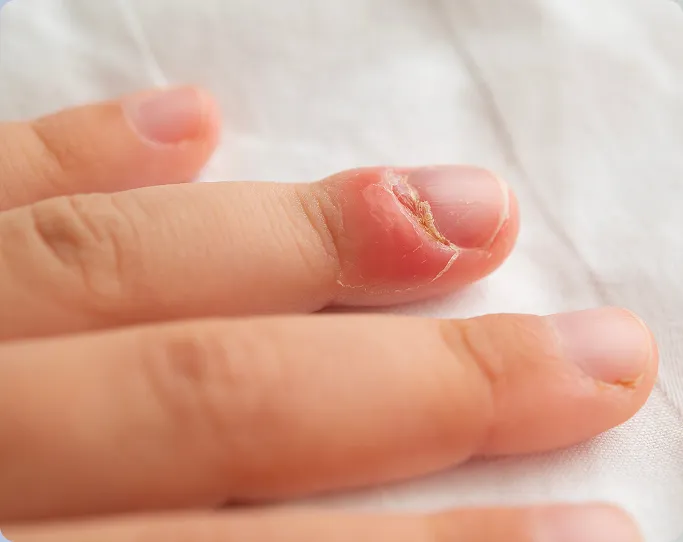
Nail conditions encompass a wide range of disorders that affect the fingernails and toenails, often serving as a window into an individual's overall health. The nail apparatus consists of the nail plate and its surrounding skin; this complex structure can be affected by various growths, infections, and structural disorders.
A healthy nail should be smooth, consistent in colour, and free of spots. However, when the nail production process is disrupted—whether by infection, trauma, or systemic disease—the nail plate can become thickened, brittle, or abnormally shaped. While most nail conditions are not life-threatening, they can cause significant physical discomfort, such as sharp pain when walking or typing, and may lead to self-consciousness. With proper diagnosis and early intervention from a dermatologist, many nail conditions can be treated effectively, restoring both the function and aesthetics of the nails.



What Is a Nail Condition?
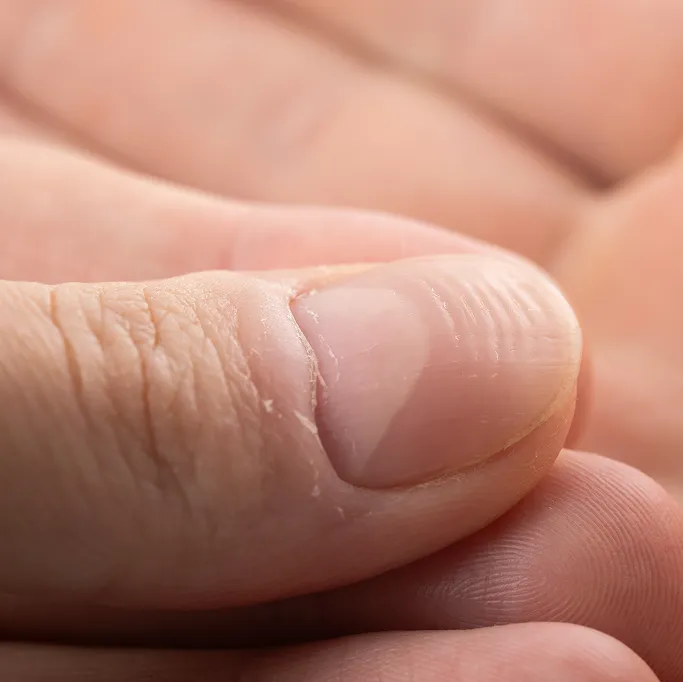
A nail condition arises when the normal growth process of the nail is disrupted. Nails are produced in the nail matrix, and any disturbance in this area—whether due to infection, trauma, or inflammation—can result in visible changes.
These changes may include thickening, discolouration, distortion, or separation from the nail bed. While minor changes like fine ridging can occur with ageing, more significant abnormalities may indicate underlying dermatological or systemic conditions and should be assessed by a specialist.
What Are Common Types of Nail Conditions?
While nails may seem uniform, nail disorders stem from a diverse array of causes—from infections and physical trauma to internal health conditions. Understanding these classifications is essential for selecting the right treatment approach.
Ingrown Nails (Onychocryptosis)
Digital Myxoid (Mucous) Cyst
Melanonychia
Fungal Nail Infection (Onychomycosis)
Common Symptoms of Nail Conditions to Look Out For
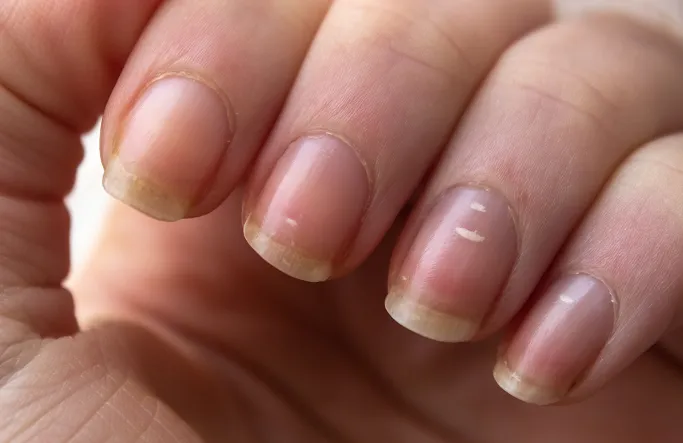
Nail conditions can present in various ways depending on the underlying cause. While some changes are mild, others may indicate infection or systemic disease.
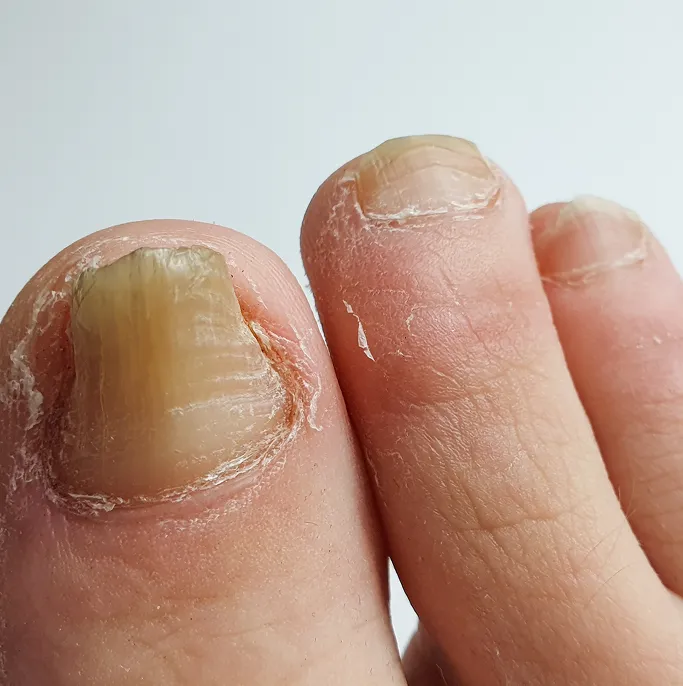
Changes in Colour
Thickening (Hyperkeratosis)
Surface Texture Irregularities
Separation from the Nail Bed (Onycholysis)
Abnormal Shape or Growth
Swelling and Inflammation
Growths Near the Nail or Joint
What Causes or Triggers Nail Conditions?
Nail conditions arise when the delicate process of nail production in the nail matrix is disrupted. Because the nail is a complex structure involving the nail plate, nail bed, and surrounding skin, various factors—both external and internal—can lead to abnormal growth or appearance.
Physical Trauma and Repetitive Stress
Improper Nail Care
Underlying Inflammatory Skin Diseases
Systemic and Metabolic Health
Joint Degeneration
Medications and Lifestyle
Genetic Predisposition
How Are Nail Conditions Diagnosed?
A dermatologist diagnoses nail conditions through a combination of medical history and clinical examination. This includes assessing the appearance of the nail plate, nail bed, and surrounding skin, as well as identifying patterns such as discolouration, thickening, pitting, or inflammation. Relevant factors such as recent trauma, footwear habits, occupational exposures, underlying skin conditions, and medications are also reviewed to determine possible causes.
Depending on the clinical findings, further investigations may be carried out to confirm the diagnosis.
Dermoscopy
Microbiological Testing
Nail Matrix Biopsy
Imaging for Underlying Structures
How Are Nail Conditions Treated at TSN Dermatology?
Treatment depends on the underlying cause and may involve medications, procedures, or supportive care to restore normal nail growth and function. Because nails grow slowly, treatment often requires consistency and follow-up to achieve visible improvement.
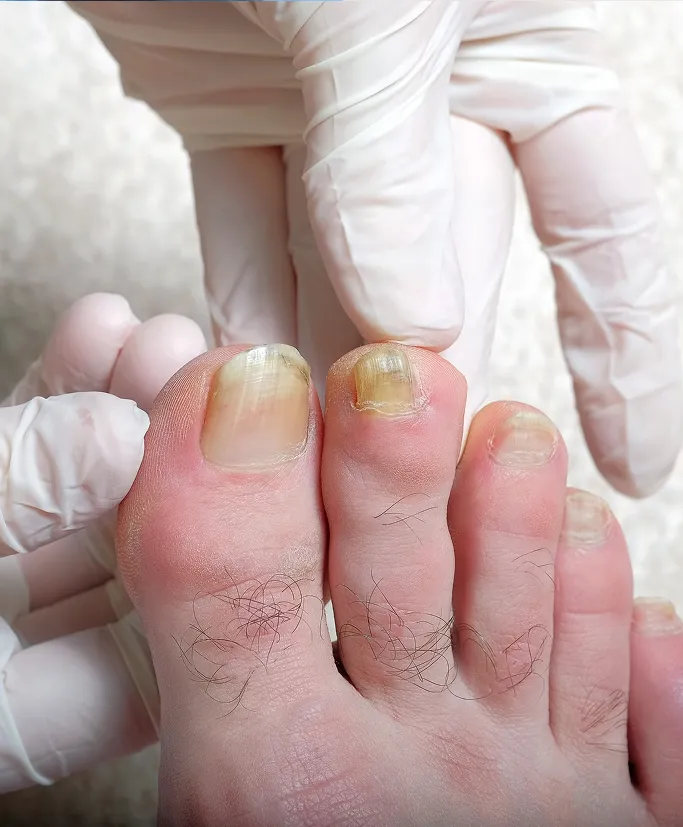
Individualised Treatment Approach
As nail conditions range from common fungal infections to inflammatory disease and structural trauma, treatment is never one-size-fits-all. Our approach is based on:
Root Cause Identification
Determining whether the nail change is due to an active infection, an inflammatory skin disorder (like psoriasis), or underlying structural issues.
Tissue Assessment
Evaluating how much of the nail plate, nail bed, and nail matrix is involved to determine the depth of treatment required.
Functional and Aesthetic Goals
Prioritising the relief of pain (e.g., in ingrown nails) while addressing the cosmetic appearance of the nail.
Long-term Monitoring
Regular follow-up is essential, as nails grow slowly; we monitor the healthy nail growth from the cuticle outward to ensure the treatment is effective.
Oral and Topical Medications
Depending on the diagnosis, medication is often the primary treatment for infectious or inflammatory nail conditions.
Oral Anti-Fungals: For chronic or deep fungal nail infections that do not respond to topicals, oral medications are the gold standard. They are typically taken for 6 to 12 weeks or longer to allow the new, healthy nail to grow out fully.
Targeted Topical Treatments: For milder infections or inflammatory conditions like nail psoriasis, specialised medicated lacquers, creams, or ointments are used to penetrate the nail plate and calm inflammation.
Procedural and Minor Surgical Interventions
For conditions involving structural distortion or persistent growths, we utilise precise in-clinic procedures:
Ingrown Nail Surgery: For severe or recurrent ingrown nails, partial nail avulsion is performed to remove only the affected portion of the nail. This may be combined with partial matricectomy to prevent the ingrown edge from recurring. Patients typically experience rapid relief once the pressure from the nail is removed.
Needle Aspiration and Injection: For digital myxoid pseudocysts, we use controlled needle aspiration to drain the fluid, often followed by the injection of medication into the area to prevent recurrence.
Cyst Management: In cases where simple aspiration is insufficient, we utilise additional treatments such as cryotherapy, laser or minor surgical excision to address the growth and relieve pressure on the underlying joint.
All procedures are performed under local anaesthesia to ensure comfort. After the procedure, patients are given appropriate wound dressings, pain relief medication and, where necessary, antibiotics to support healing and reduce discomfort.
Supportive Care and Maintenance
Protective Advice: Guidance on proper footwear, nail trimming techniques, and avoiding aggressive cuticle manipulation to prevent recurrence of ingrown nails or trauma-related dystrophy.
Preventative Protocols: Strategies to maintain a healthy nail environment, especially for patients prone to fungal infections or those with systemic health issues that affect nail integrity.
Tips on Daily Nail Care and Prevention
For individuals prone to nail conditions, consistent daily care is essential. Whether you are recovering from a fungal infection, managing a structural deformity, or prone to painful ingrown nails, these habits help minimise damage and maintain the health of your nail matrix and nail bed.
Proper Nail Grooming Techniques
-
Trim Nails Straight Across
Avoid rounding the corners too deeply, as this is a primary cause of ingrown nails. Use a clean, sharp nail clipper to keep the nail edge straight and just level with the tip of your toe or finger. -
Do Not Dig at Corners
Resist the urge to perform bathroom surgery on an ingrown nail. Digging into the nail fold can breach the skin, introducing bacteria and leading to painful infections. -
Gentle Cuticle Care
Never aggressively cut or push back your cuticles. The cuticle acts as a vital seal protecting the nail matrix from pathogens. Damaging this seal is a common trigger for paronychia and chronic nail inflammation.
Protection and Hygiene
-
Keep Feet Dry
Fungal spores thrive in warm, dark, moist environments. After bathing, thoroughly dry the skin between your toes. If you are prone to sweating, change your socks during the day and ensure your shoes are fully dry before wearing them again. -
Wear Protective Footwear
In communal areas like swimming pools, gyms, and public showers, always wear shower sandals. This simple habit is the most effective way to prevent the transmission of fungal nail infections. -
Choose Proper Footwear
Wear shoes with a wide toe box that do not compress your toes. Tight, pointy shoes exert continuous mechanical pressure on the nail plate, which is a leading trigger for ingrown nails and nail bed distortion.
Monitor for Early Signs of Infection
-
Check for Micro-changes
Look for subtle signs such as small white spots, a slight thickening of the nail, or the nail starting to lift (onycholysis). Fungal infections are significantly easier to treat when caught early, before the fungus reaches the nail matrix. -
Watch for Redness or Swelling
If you notice redness, warmth, or throbbing around the nail fold, it is a warning sign of an acute infection. Do not wait for pus to develop; seek professional advice to address the inflammation early.
Environmental and Lifestyle Factors
-
Use Gloves for Chemical Exposure
If your hands are frequently in water, or if you work with detergents, harsh solvents, or cleaning chemicals, wear protective rubber gloves. Chemical exposure can strip the nail of its protective oils, leading to brittleness and peeling. -
Balanced Nutrition
A healthy nail plate requires adequate protein, vitamins, and minerals. A balanced diet supports the nail matrix in producing strong, healthy keratin, which is essential for resilient nails.
Proactive Management
-
Do Not Ignore Discolouration
If you notice a dark or brown band appearing on your nail (melanonychia), do not dismiss it as a bruise or stain. Have it evaluated by a dermatologist using a dermatoscope to ensure it is not a sign of subungual melanoma. -
Follow Treatment Courses
Nail treatments, particularly for fungus, take a long time because the nail grows slowly. If prescribed a long course of medication, remain consistent. Prematurely stopping treatment is the most common reason for persistent or recurring nail infections.



When Should You See a Dermatologist for Nail Conditions?
While minor nail issues like a single hangnail or simple bruising often resolve on their own, the nail unit is a complex structure where subtle changes can indicate underlying infections, chronic skin conditions, or systemic disease. You should schedule a consultation with a dermatologist if you experience any of the following:
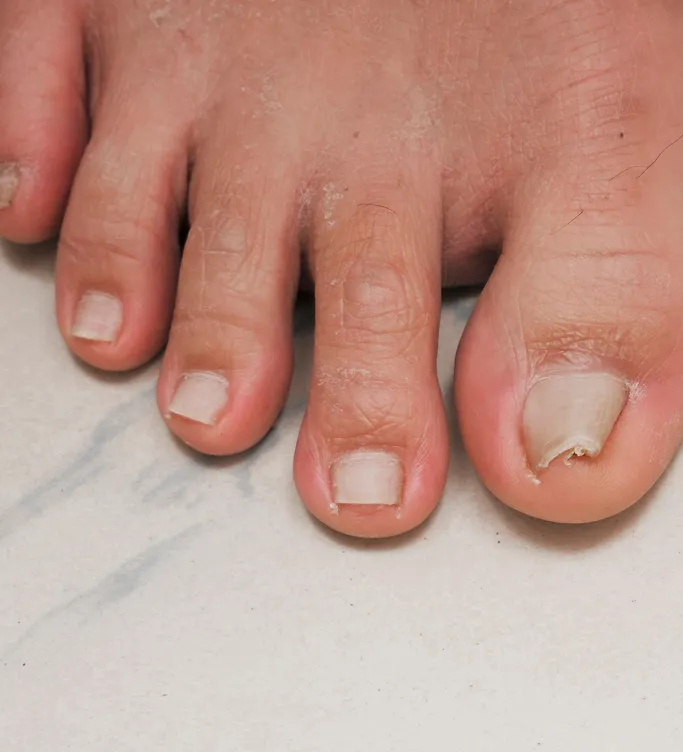
Sudden or Persistent Pigmentation Changes
If you notice a new brown, black, or grey band running down your nail (melanonychia) that wasn't there before, it requires professional evaluation. While often benign, a dermatologist must use a dermatoscope to rule out subungual melanoma, an aggressive form of skin cancer that can mimic simple bruising or fungal staining.
Signs of Chronic Infection
If you notice persistent redness, swelling, or the discharge of pus from the skin fold around the nail (paronychia), or if your nail is thickening, crumbling, or separating from the nail bed, you may have a fungal infection. These conditions rarely improve with over-the-counter creams and require medical confirmation via laboratory testing for proper oral treatment.
Painful Ingrown Nails
If an ingrown nail is causing persistent pain, bleeding, or signs of secondary infection (like pus), do not attempt bathroom surgery. A dermatologist can provide safe, effective relief—often through minor surgical procedures—that addresses the root cause and prevents the infection from worsening or spreading to the underlying bone.
Unusual Growths or Cysts
If you develop a small, dome-shaped, or translucent growth near the cuticle or the joint of your finger, it could be a digital myxoid pseudocyst. These are often linked to joint degeneration and can become painful or lead to nail deformity if left unaddressed.
Progressive Nail Distortion
If your nails are becoming increasingly brittle, spoon-shaped (koilonychia), heavily ridged, or are separating from the nail bed (onycholysis) without a clear history of trauma, it may signal an underlying systemic condition, such as anaemia, thyroid dysfunction, or inflammatory skin disease like psoriasis.
Failure to Respond to Home Care
If you have been treating a suspected issue at home for several weeks with no improvement, it is time for a professional assessment. Because nails grow very slowly, waiting months for an ineffective treatment to work can allow a condition—like a fungal infection or nail dystrophy—to become much more difficult and costly to treat later.
FAQs About Nail Conditions
Yes. Fungal infections of the nail can be transmitted through contact with infected skin scales or nail debris in communal areas like swimming pools, gym showers, and locker rooms. Sharing personal items like nail clippers or towels with an infected person can also facilitate the spread.
For an ingrown nail, partial nail removal performed by a professional can provide relief and correct the growth. However, for fungal infections or nail psoriasis, simply trimming the visible bad nail does not treat the underlying disease within the nail matrix. The nail will likely continue to grow back in an unhealthy state until the root cause is medically treated.
Nails grow very slowly—fingernails typically take 4 to 6 months to grow out fully, and toenails can take 12 to 18 months. Treatment for conditions like fungal infections or psoriasis is not instantaneous; you are essentially waiting for the new, healthy nail to grow from the cuticle and replace the old, damaged portion. Consistency is key, even when you don't see immediate changes.
While it may be tempting to cover discoloured or thickened nails, wearing polish for long periods can trap moisture and worsen fungal infections or conceal signs of progression. If you must use polish, choose a breathable formulation, ensure the nail is completely clean and dry before application, and avoid leaving it on for extended periods. If you have a suspected pigment change, avoid polish entirely until a dermatologist has evaluated it with a dermatoscope.
Many home remedies, such as vinegar soaks or tea tree oil, are often cited online. While some have mild antiseptic properties, they rarely penetrate deep enough into the nail plate to reach the infection site in the nail bed. Relying solely on home remedies can delay effective medical treatment, allowing the infection to spread to other nails or deeper into the nail matrix.
Yes. Because the nail matrix is sensitive to systemic health, changes in your nails can sometimes be the first physical indicator of underlying issues like anaemia, thyroid disorders, or nutritional deficiencies. If your dermatologist notices abnormal nail patterns across multiple fingers or toes, they may suggest blood tests to investigate your overall internal health.
Seek Proper Dermatologist Care for Nail Conditions
If you notice persistent or unusual changes in your nails, a consultation with our dermatologists at TSN Dermatology Skin Specialist Clinic can help establish an accurate diagnosis and guide appropriate management. Contact us for more information or to arrange an appointment.
Meet TheDoctors Behind Your Care

Dr Koh Hong Yi
Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in treatment for nail conditions, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh