Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
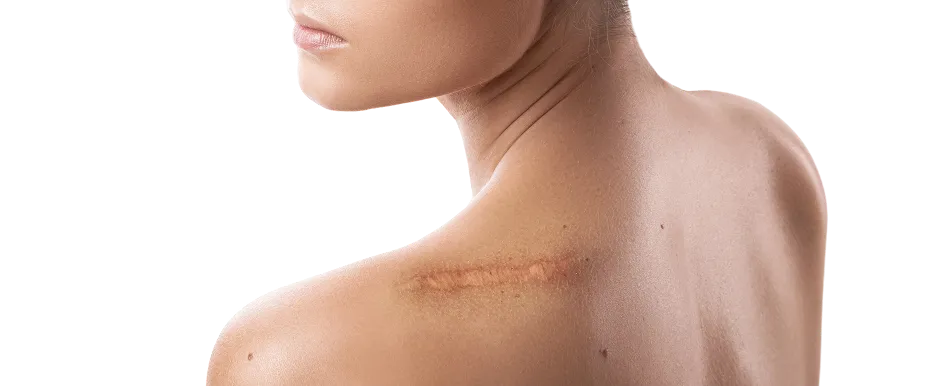
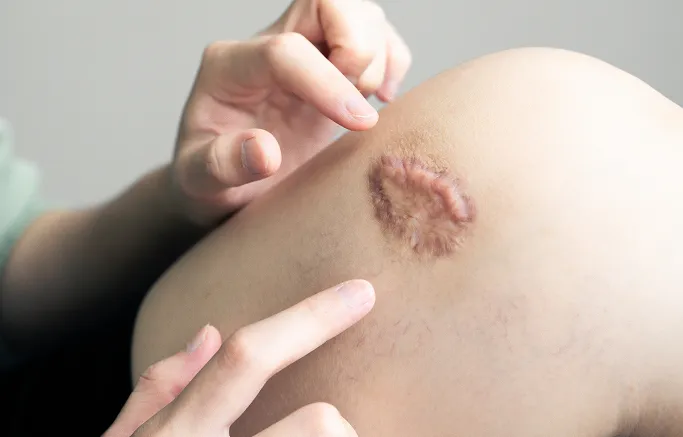
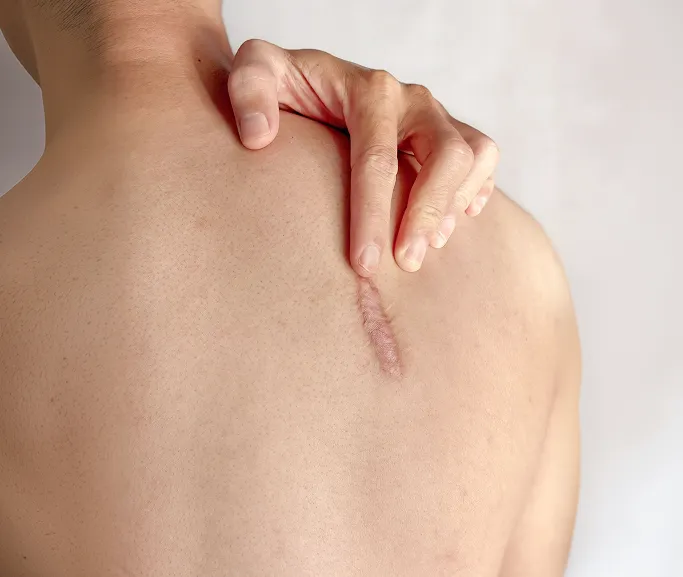
A keloid is a type of raised scar that occurs when the body produces too much collagen during the healing process after a skin injury. Unlike normal scars, keloids extend beyond the boundaries of the original wound and do not typically regress over time. They are often firm, rubbery, and can vary in colour from flesh-toned to red or dark brown.
Although keloids are benign, they can cause significant physical discomfort, pain, or itchiness, and may lead to self-consciousness or anxiety regarding appearance. With proper diagnosis and early intervention from a dermatologist, keloids can be flattened, softened, and managed effectively to improve comfort and aesthetics.



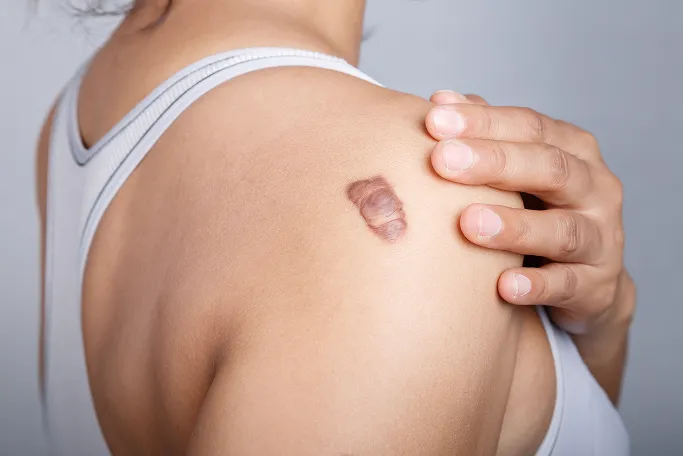
What Is a Keloid?
A keloid is a result of an overactive healing response. When the skin is injured, the body produces collagen to repair the damage. In keloid-prone individuals, this process continues excessively, causing the scar tissue to grow uncontrollably and spread into the surrounding healthy skin.
A keloid is not simply a raised scar (hypertrophic scar). It is a distinct fibroproliferative disorder. While hypertrophic scars stay within the original wound area, keloids grow outward, which is why specialised dermatological care is required to prevent further expansion and address symptoms like pain or restricted movement.
What Are Common Classifications of Keloid Scars?
While all keloids stem from excessive collagen deposition, they are often categorised based on their origin and clinical behaviour. Understanding these classifications is essential for selecting the right treatment approach.
Spontaneous Keloids
Burn-Related Keloids
Traumatic Keloids
The most common form develops after physical trauma to the skin.
-
Surgical Keloids
Frequently occur along incision lines following procedures like C-sections, cardiac surgery, or minor excisions. -
Piercing and Tattoo-Related Keloids
Commonly seen on the earlobes due to trauma from piercings, often requiring a combination of surgical excision and serial steroid injections to prevent recurrence.
Keloids on High-Tension Sites
Acne-Induced Keloids
Recurrent Keloids
Common Symptoms of Keloids to Look Out For
Keloids can present differently depending on their age and size. While some are asymptomatic, others cause chronic issues. The following are some of the most common signs patients may experience.
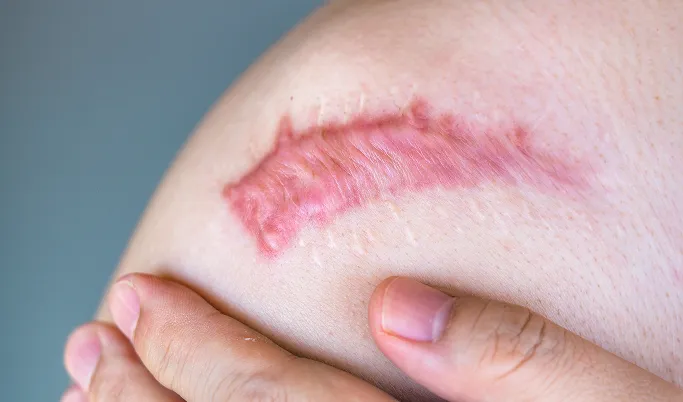
Raised and Firm Texture
Overgrowth Beyond Wound Edges
Itching and Pain
Colour Variations
Texture and Irregularity
Restricted Movement
What Causes or Triggers Keloid Formation?
Keloids occur when the normal wound healing process goes into overdrive. While the exact trigger isn't always identifiable, the following are recognised contributors.
Skin Trauma
Piercings and Tattoos
Genetic Predisposition
Skin Tension
Inflammation
Age and Skin Pigmentation
How Are Keloids Diagnosed?
Accurate diagnosis is crucial, as other skin conditions or even certain types of skin tumours can sometimes mimic keloids. A dermatologist will typically assess a suspected keloid using the following methods:
Clinical Examination
Medical History Review
Assessment of Symptom Profile
Exclusion of Other Conditions
Skin Biopsy
How Are Keloid Scars Treated at TSN Dermatology?
Effective management of keloid scars requires a multi-modal strategy that combines physical, medical, and procedural interventions. Because keloids are complex fibroproliferative growths rather than simple scars, we provide personalised treatment plans tailored to the size, maturity, and location of the lesion.
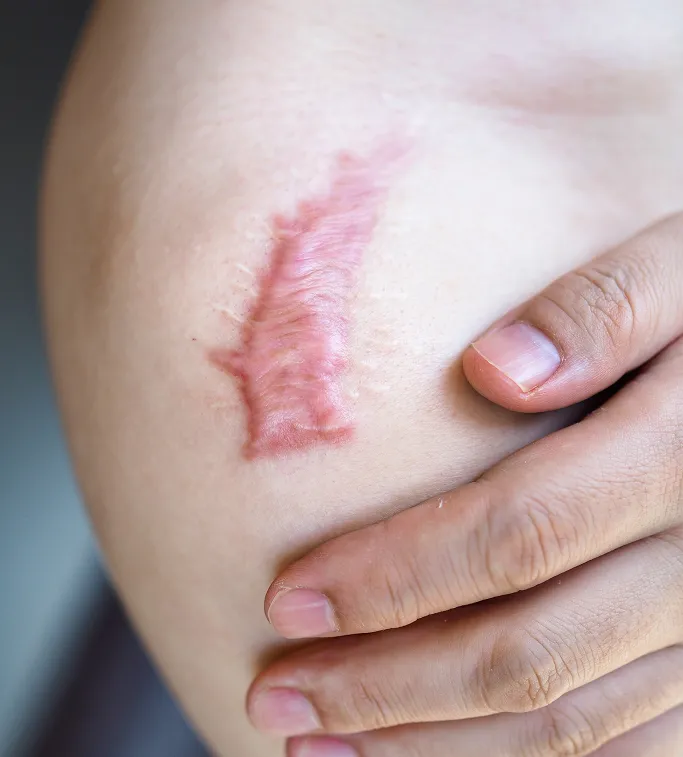
Individualised Treatment Approach
As keloids vary significantly in their growth patterns and response to therapy, treatment is never one-size-fits-all. Our approach is based on:
Scar Assessment
Evaluating the thickness, vascularity (redness), and location of the keloid to determine the best combination of therapies.
Risk of Recurrence
Considering your past history and family predisposition, which informs our choice of adjuvant (add-on) treatments to prevent the scar from regrowing.
Functional Impact
Assessing if the scar causes pain, itch, or restricts movement near joints.
Long-term Monitoring
Regular follow-up to ensure the scar remains flattened and to adjust the regimen as the tissue matures.
Intralesional Injections
Steroid injection into the scar is the most common and effective treatment. This helps to flatten the scar, stop it from growing further, and significantly reduces the itch or pain associated with the tissue.
Safety Profile: The amount of steroid absorbed by the rest of the body is kept to a minimum, as the medication is concentrated precisely within the scar tissue.
Treatment Schedule: Injections typically need to be repeated every one to a few months until a desirable, flattened outcome is achieved.
Procedural Therapies
For keloids that are resistant to injections alone, we utilise advanced procedural techniques:
Cryotherapy: Using liquid nitrogen to freeze the tissue, which helps destroy the excessive collagen fibres and shrink the scar.
Laser Therapy: Pulsed-dye or vascular lasers can be used in selective situations to target the blood vessels feeding the keloid, effectively reducing the redness and thickness of the scar.
Surgical Excision: For certain locations, such as the earlobe, keloids may be amenable to surgical removal. Crucially, this is typically combined with post-surgical treatments, such as steroid injections, to reduce the risk of recurrence.
Topical and Non-Invasive Care
Silicone Gel Sheets: These are a non-invasive treatment option that can help improve scar hydration and support overall scar management. They provide a protective barrier that hydrates the scar and regulates collagen production. This is particularly useful for early-stage scars or as a maintenance therapy following other procedures.
Tips on Daily Keloid Care and Prevention
For individuals prone to keloid formation, diligent daily care is essential. While you cannot always prevent a keloid from forming if you are genetically predisposed, these habits help minimise inflammation and keep existing scars manageable.
Gentle Skin Handling and Protection
-
Avoid Unnecessary Trauma
Be cautious with your skin. Avoid elective procedures like new piercings, tattoos, or minor cosmetic surgeries if you have a known history of keloid formation, as these are common triggers for abnormal scarring. -
Sun Protection
Keep your scars protected from the sun. UV rays can cause post-inflammatory hyperpigmentation, making the keloid darker and more noticeable. Use a high-SPF sunscreen or keep the area covered when outdoors. -
Moisturise Gently
Keep the skin around the scar hydrated with fragrance-free, hypoallergenic moisturisers to maintain a healthy skin barrier, but avoid aggressive rubbing or scrubbing of the scar itself.
Consistent Silicone and Pressure Therapy
-
Early Application
If you have a healing wound, start using silicone gel or silicone sheets as soon as the skin has closed. This creates an optimal environment that hydrates the tissue and regulates collagen production, which can help prevent a normal scar from evolving into a keloid. -
Pressure Garments
In selected cases, particularly after procedures or in high-risk scars, pressure therapy may be recommended.. Continuous, gentle pressure helps to flatten the tissue and can be a powerful tool in keeping a keloid from thickening.
Trigger Identification and Management
-
Monitor for Inflammation
Keloids thrive on inflammation. If you notice a scar suddenly becoming redder, itchier, or more painful, it is a warning sign that the keloid is active. Do not wait for it to grow; seek professional advice to calm the inflammation. -
Manage Acne and Rashes
If you are prone to keloids on your chest or back, aggressive management of inflammatory conditions like acne is crucial. Using medicated washes to prevent acne outbreaks can stop keloids from developing in the first place.
Itch Control and Skin Protection
-
Do Not Scratch
Scratching a keloid can introduce bacteria and create micro-trauma, which stimulates further collagen growth. If the keloid is itchy, apply a cold compress or a dermatologist-prescribed soothing lotion rather than scratching the surface. -
Avoid Tight Clothing
Wear loose-fitting, soft fabrics in areas where you have keloids to reduce friction and mechanical tension, as constant rubbing can increase the thickness of the scar.
Environmental and Lifestyle Factors
-
Keep the Area Cool
In Singapore's hot and humid climate, excessive sweat can irritate the skin surrounding a keloid and worsen the itch. Shower promptly after exercise and keep the area dry to prevent maceration or secondary irritation. -
Stress Reduction
While stress does not directly cause a keloid, chronic stress can impact immune function and the body's inflammatory response. Maintaining your overall health helps support the skin's ability to manage its healing processes properly.
Early Management and Proactive Care
-
Be Proactive
If you notice a scar starting to thicken or grow beyond the original site of injury, do not ignore it. Early intervention with intralesional steroids is far more effective at stopping a keloid's growth than trying to remove a large, mature, and hardened scar later.



When Should You See a Dermatologist for Keloid Scars?
While some small scars may be manageable, keloids are fibroproliferative growths that often require professional medical intervention to stop their progression. You should schedule a consultation with a dermatologist if you experience any of the following:
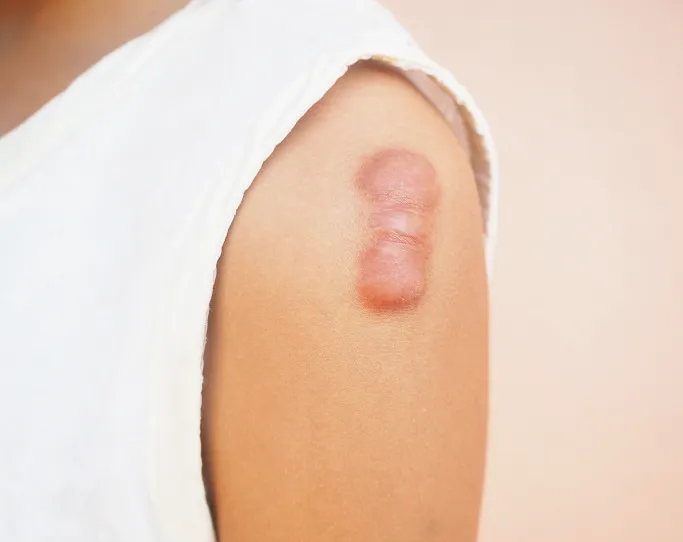
Rapid or Persistent Growth
If you notice a scar is visibly increasing in size, thickness, or claw-like expansion over several months, it indicates an active keloid process that needs early medical suppression.
Chronic Pain or Intolerable Itching
If the scar causes persistent, nagging itching, tenderness, or sharp pain that impacts your quality of life, a dermatologist can provide treatments to calm the internal inflammation of the tissue.
Functional Limitation
If the keloid is located near a joint (such as the shoulder, elbow, or neck) and is creating enough tension to restrict your natural range of motion or pulling on your skin, it requires professional assessment for reduction.
Family History Concerns
If you have a strong genetic predisposition (a family history of keloids) and are considering any elective surgical, cosmetic, or piercing procedures, consult us first. We can discuss preventative measures to ensure your skin does not develop abnormal scarring.
Signs of Recurrence
If you have previously had a scar removed (surgically or otherwise) and it has begun to grow back, do not wait. Recurrent keloids can be more aggressive, and early intervention is vital to regain control.
Uncertainty About the Lesion
If a growth on your skin is raised, firm, or changing in colour, but you are unsure if it is a keloid, a professional diagnosis is necessary to rule out other skin conditions or rare tumours that may mimic keloid appearance.
FAQs About Keloid Scars
No. Keloids are not contagious and cannot be spread through physical contact, sharing personal items, or close interaction with others. They are an internal, fibroproliferative response within your own skin's collagen-producing cells.
Keloids are challenging to manage because they have a high tendency to recur. While there is no cure that makes a mature keloid disappear instantly, consistent professional treatment can flatten, soften, and significantly improve the appearance and comfort of the scar, keeping it in long-term remission.
Surgery is not typically the first line of treatment. Because the act of cutting the skin can trigger an even more aggressive inflammatory response, surgery alone has a very high risk of recurrence. Surgery is usually reserved for specific locations (like the earlobe) and must be combined with adjuvant therapies, such as post-surgical steroid injections, to prevent the keloid from returning.
Keloid formation is often linked to a genetic predisposition. Some individuals have a unique biological response where their skin does not know when to stop producing collagen after an injury. If you have a family history of keloids, your skin is more likely to develop these abnormal scars even from minor injuries like acne or small cuts.
Generally, no. Unlike normal scars that may fade and flatten over time, keloids are characterised by their inability to regress naturally. Without professional medical intervention, keloids often remain stable or continue to grow slowly over many years.
There is no evidence that specific foods cause or prevent keloids. However, maintaining a healthy, balanced diet supports overall skin health and immune function, which is beneficial for the body's natural healing processes following any injury or dermatological procedure.
Seek Proper Dermatologist Care for Keloid Scars
If you or your child have developed keloid scars, a consultation with our specialists at TSN Dermatology Skin Specialist Clinic can help clarify the diagnosis and establish an effective, personalised treatment plan focused on long-term skin health and quality of life. For more information or appointments, please contact us today.
Meet TheDoctors Behind Your Care

Dr Koh Hong Yi
Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in keloid treatment, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh