Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
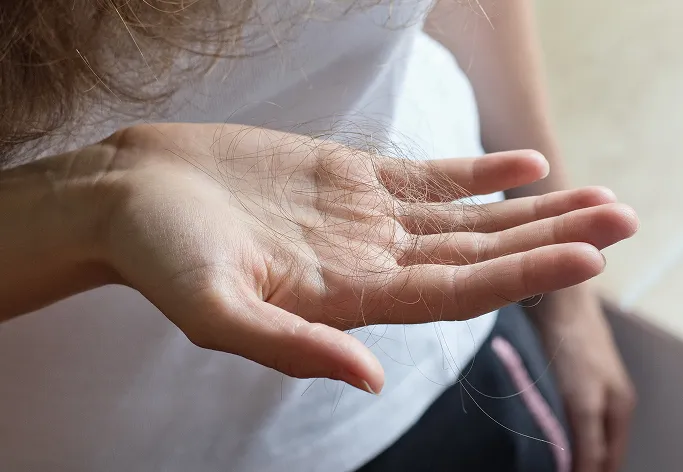
Hair loss is a common condition that affects both men and women, often causing significant emotional distress and impacting self-confidence. It is characterised by thinning hair, a receding hairline, or the emergence of bald patches on the scalp. While hair loss can be a natural part of ageing, it may also be an indicator of underlying medical issues, hormonal changes, or genetic predispositions.
Although not all forms of hair loss can be fully reversed, many types can be effectively managed, slowed, or even treated with accurate diagnosis, personalised interventions, and long-term scalp care under the guidance of a dermatologist.




What Is Hair Loss?
Hair loss, or alopecia, occurs when the hair growth cycle is disrupted. Normally, hair grows in phases: a growth phase, a transition phase, and a resting phase, followed by shedding. Hair loss happens when this cycle is shortened, when hair follicles become dormant, or when the follicles are damaged and replaced by scar tissue.
Hair loss is not just a cosmetic concern; it is a clinical condition that requires professional assessment. Whether triggered by genetics, immune system activity, or systemic health, understanding the specific mechanism behind the hair loss is essential for choosing an effective treatment path.
What Are Common Types of Hair Loss?
There are several types of hair loss, and a precise diagnosis is crucial for selecting the appropriate therapy.
Androgenetic Alopecia
- The most common form of hair loss is often called male or female pattern hair loss.
- In men, it typically presents as a receding hairline and thinning at the crown; in women, it usually manifests as diffuse thinning along the central parting.
- Driven by a combination of genetics and the sensitivity of hair follicles to androgens (hormones).
- Treatment depends on the severity of the condition and the expectations of the patient. Options include topical lotions (e.g., minoxidil), oral medications (e.g., finasteride, minoxidil) and hair transplantation.
Traction Alopecia
- Caused by repetitive tension or pulling on the hair shafts, often due to tight hairstyles like braids, buns, or extensions.
- Typically affects the hairline or temples and can lead to permanent damage if the tension is not relieved.
- Prevention is key, as chronic traction can lead to permanent follicle scarring.
Telogen Effluvium
- A temporary form of hair loss characterised by excessive shedding, often occurring after a significant physiological stressor.
- Triggers can include childbirth, severe illness, rapid weight loss, major surgery, or intense emotional stress.
- Usually reversible once the underlying trigger is addressed and the body recovers.
Anagen Effluvium
- Sudden, widespread hair loss that occurs during the active growth phase of hair.
- Most commonly associated with medical treatments like chemotherapy, which temporarily halts the rapid division of hair follicle cells.
- Hair growth usually resumes after the cessation of the triggering treatment.
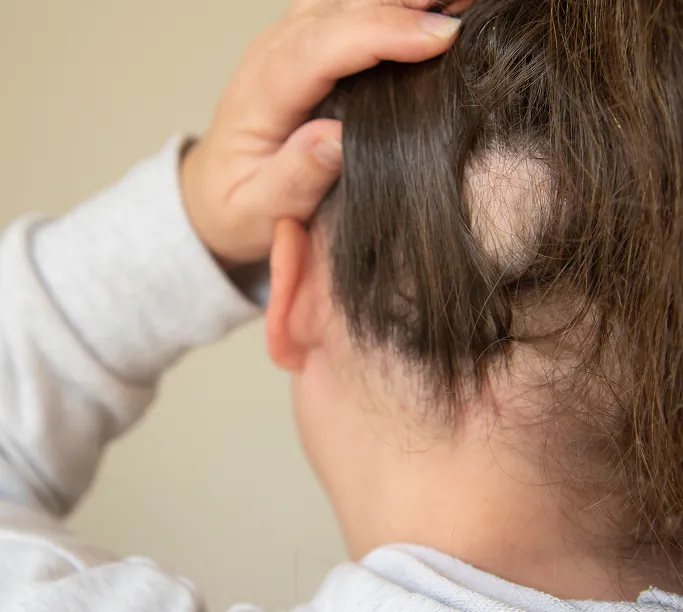
Alopecia Areata
- An autoimmune condition where the body's immune system mistakenly attacks hair follicles, leading to sudden, patchy hair loss.
- Patches are typically smooth, round, and may appear on the scalp, beard area, or eyebrows.
- The condition is unpredictable and may range from small, self-resolving patches to complete scalp or body hair loss.
- Treatment includes topical lotions, injections, immunotherapy and oral medications. Some of the latest treatments include JAK/STAT inhibitors (e.g., tofacitinib), which have been useful in patients with more severe disease.
Cicatricial (Scarring) Alopecia
- A group of inflammatory conditions that cause permanent destruction of hair follicles and replace them with scar tissue.
- Early diagnosis is critical to stop the inflammation before the hair loss becomes irreversible.
- May present with redness, scaling, or burning sensations on the scalp.
Common Symptoms of Hair Loss to Look Out For
Hair loss, also known as alopecia, can manifest in various ways depending on the underlying cause. While it is normal for most people to shed between 50 and 100 hairs per day, excessive shedding or thinning indicates an issue. Symptoms can appear in localised patches, diffusely across the whole scalp, or in specific patterns.

Increased Daily Shedding
Gradual Thinning
Receding Hairline
Patchy Baldness
Scalp Irritation
Diffuse Thinning
Visible Scalp Through Thinning Hair
What Triggers Hair Loss or Increased Shedding?
While some forms of hair loss are genetic, others are triggered by systemic stress or environmental factors that disrupt the normal hair growth cycle. Recognising these triggers is the first step toward effective management and, in many cases, recovery.
Physical and Emotional Stress
Significant stress to the body is a primary trigger for telogen effluvium. This form of diffuse hair loss is often preceded by stressful life events such as childbirth, severe illness, hospitalisation, or rapid weight loss, which can temporarily shift hair follicles into a resting and shedding phase.
Hormonal Imbalances
Fluctuations in hormones, whether due to thyroid conditions, pregnancy, menopause, or underlying endocrine disorders, can significantly disrupt hair growth, often leading to diffuse thinning.
Genetics and Family History
Hereditary factors are the leading cause of androgenetic alopecia. If you have a family history of balding or hair thinning, your follicles may be more sensitive to hormonal changes, leading to patterned loss over time.
Immune System Reactions
In conditions like alopecia areata, the body's immune system mistakenly identifies its own hair follicles as foreign threats, triggering an inflammatory response that leads to sudden, localised, circular patches of hair loss.
Medications
Certain prescription drugs can act as triggers for diffuse hair shedding. If you notice a sudden change in hair density after starting a new medication, it is important to discuss this with your dermatologist.
Nutritional Deficiencies
Hair follicle cells are some of the most rapidly dividing in the body. A lack of essential nutrients, such as iron, vitamin D, B vitamins, or proteins, can weaken the hair shaft or prematurely halt the growth cycle.
Hairstyling Habits and Tension
Excessive pulling, tight hairstyles (like braids, buns, or extensions), and harsh chemical treatments or high-heat styling can cause mechanical damage. This can lead to traction alopecia, where the follicle is damaged over time due to constant tension.
How Is Hair Loss Diagnosed?
Accurate diagnosis is essential, as the underlying cause of hair loss, whether it be hormonal, immune-mediated, or due to stress, determines the most effective treatment plan. A dermatologist will typically assess hair loss using the following methods:
Clinical Examination
Medical History Review
Pull Test
Dermoscopy
Blood Tests
Scalp Biopsy
How is Hair Loss Treated at TSN Dermatology?
Effective hair loss management requires an individualised treatment plan tailored to the specific type of alopecia, the severity of the condition, and the patient's expectations. Because hair follicles grow in cycles, treatments are designed to stimulate growth, prolong the growth phase, or address the underlying cause of shedding.

Individualised Treatment Approach
Treatment plans are customised based on:
The type of alopecia diagnosed (e.g., androgenetic, alopecia areata, or telogen effluvium)
The extent and duration of hair loss
Whether the condition is inflammatory or scarring
The patient's medical history and current lifestyle
Topical and Oral Treatments
Medications are often the first line of defence to stimulate follicles and prevent further loss.
Topical therapies
Solutions like minoxidil are commonly used to improve blood flow to the hair follicles and extend the active growth phase.
Oral medications
Treatments such as finasteride or oral minoxidil may be prescribed to target the hormonal factors driving androgenetic alopecia.
Targeted therapy
For patients with severe alopecia areata, the latest treatments include JAK/STAT inhibitors (e.g., tofacitinib). These advanced medications work by blocking specific signalling pathways that cause the immune system to attack hair follicles.
Scalp Injections and Regenerative Procedures
For patients seeking to rejuvenate dormant follicles, we offer procedural interventions.
Injections: Corticosteroid injections are frequently used to treat the patches associated with alopecia areata by calming the local immune response.
Platelet-Rich Plasma (PRP) Therapy: This involves concentrating growth factors from your own blood and injecting them into the scalp to stimulate hair density and follicle health.
Microneedling: Often used in combination with topical treatments to enhance absorption and stimulate the skin's natural repair process.
Surgical Hair Transplantation
For patients with permanent hair loss or androgenetic alopecia that has not responded adequately to medical therapy, hair transplantation may be considered. This involves moving healthy, DHT-resistant hair follicles from the back or sides of the scalp to areas with thinning or balding. This procedure is performed with precision to ensure natural-looking density and requires careful pre-surgical planning.
Tips on Daily Hair Care and Hair Loss Prevention
Consistent scalp care and mindful styling habits are key to maintaining follicle health and preventing further hair loss. While not all hair loss can be prevented, these habits help create the best possible environment for hair growth.
Gentle Cleansing and Handling
Minimise Tension
Scalp Health and Hygiene
Sun and Environmental Protection
Manage Stress
Careful Styling and Heat Usage
Early Intervention



When Should You See a Dermatologist for Hair Loss?
Hair loss can be a complex issue, and early intervention is often the most critical factor in achieving successful long-term outcomes. You should consider booking a consultation with a dermatologist if you experience any of the following:

Sudden or Unexplained Shedding
If you notice a sudden increase in hair loss, losing large amounts of hair while showering, brushing, or waking up, this could be a sign of telogen effluvium or other systemic issues that require professional evaluation to identify the trigger.
Patchy Hair Loss
The appearance of circular, coin-shaped patches on your scalp, beard, or eyebrows is a key indicator of alopecia areata. Because this condition is driven by the immune system, early medical intervention with injections or specialised topical therapies is vital.
Noticeable Thinning or Receding Hairline
If you observe a widening part line, thinning at the crown of your head, or a receding hairline, these are classic signs of androgenetic alopecia. These conditions are often progressive, and starting treatment early can help preserve your existing hair and slow further loss.
Scalp Discomfort or Inflammation
If your hair loss is accompanied by scalp redness, persistent itching, burning, scaling, or pain, you may be dealing with an inflammatory or scarring form of alopecia. In these cases, prompt medical treatment is required to prevent permanent damage to the hair follicles.
Failure of Over-the-Counter Products
If you have been using shampoos or supplements marketed for hair growth for several months without seeing any improvement, it is time to seek professional advice. A dermatologist can provide evidence-based treatments, such as minoxidil, finasteride, or JAK/STAT inhibitors, that are tailored to your specific diagnosis.
Concern Regarding Family History
If you have a strong family history of hair loss and are concerned about your own risk, a dermatologist can provide a proactive assessment and discuss preventative strategies before significant thinning occurs.
FAQs About Hair Loss
No. Hair loss, including autoimmune types like alopecia areata, is not contagious. It cannot be spread through physical contact, sharing personal items, or close interaction with others.
While some forms of hair loss, such as telogen effluvium, often resolve spontaneously once the trigger is removed, others, such as androgenetic alopecia, are chronic and progressive. While they may not have a cure in the sense of total reversal, consistent, evidence-based management can significantly slow the progression, restore density, and help patients achieve excellent long-term control.
When used under professional dermatological guidance, treatments such as minoxidil, finasteride, and JAK/STAT inhibitors (like tofacitinib) are safe and effective. As with any medical intervention, risks and side effects should be discussed with your dermatologist to ensure the chosen treatment is appropriate for your specific health profile.
A balanced diet is crucial for healthy hair growth. While specific nutritional deficiencies (like low iron or Vitamin D) can trigger hair shedding, supplements are generally only effective if there is a documented deficiency. They should not be used as a substitute for professional diagnosis, as they will not stop pattern or immune-mediated hair loss.
Stress typically triggers telogen effluvium, a temporary form of hair loss where follicles enter a resting phase. While the shedding can be alarming, it is usually not permanent, and hair typically begins to regrow once the stressful period subsides or is managed.
Not necessarily. Hair transplantation is a surgical option primarily for patients with stable, pattern-based hair loss who have a sufficient donor area of healthy follicles. It is not suitable for patients with active inflammatory or scarring hair loss, which is why a thorough dermatological assessment is required before considering any surgical procedure.
Seek Proper Dermatologist Care for Hair Loss
If you or your child are experiencing persistent or worsening hair loss, a consultation with our specialists at TSN Dermatology Skin Specialist Clinic can help clarify the diagnosis and establish an effective, personalised treatment plan focused on long-term skin health and quality of life. For more information or appointments, please contact us today.
Meet TheDoctors Behind Your Care

Dr Koh Hong Yi
Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in hair loss treatment, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh