Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
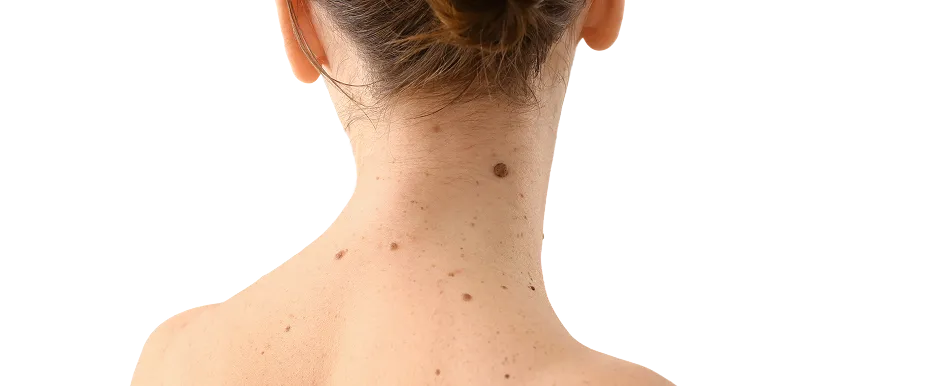
A benign skin growth is a non-cancerous lesion that arises from the skin's various cell types, such as epidermal cells, pigment cells, blood vessels, or connective tissue. Unlike malignant skin tumours, benign growths do not invade surrounding tissues in the same way as malignant tumours or spread to other parts of the body (metastasise). While they are typically harmless in terms of physical health, they can often be a source of cosmetic concern, irritation, or anxiety if their appearance changes or if they interfere with daily activities.
With professional dermatological assessment, many benign growths can be accurately identified, monitored, or safely removed to improve comfort and aesthetics.



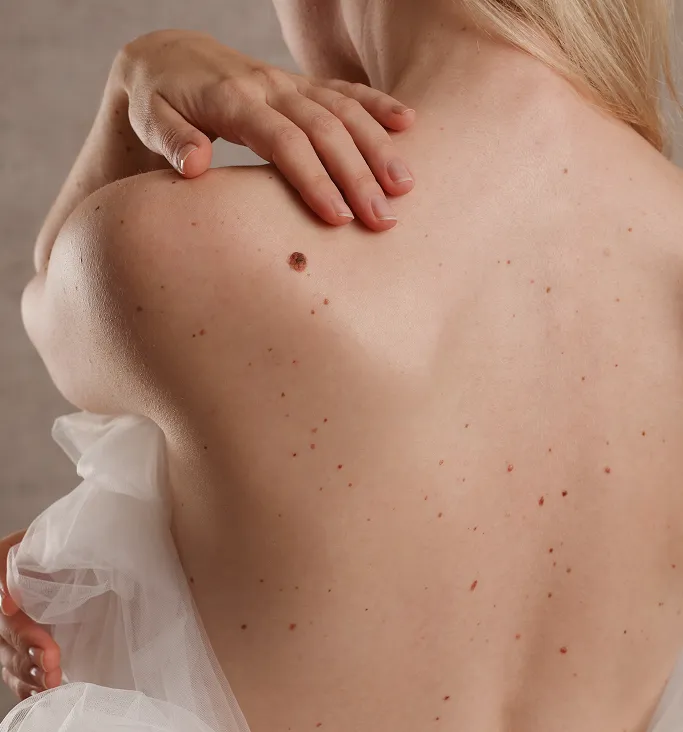
What Is Benign Skin Growth?
A benign skin growth is an overgrowth of normal skin cells that form a localised lesion. While the cause varies depending on the type, ranging from sun damage and ageing to genetic predisposition or viral triggers, the defining characteristic is that the growth remains localised and does not spread to other parts of the body, although some may increase in size over time.
Common examples of benign growths include seborrheic keratoses, skin tags, cherry angiomas, and dermatofibromas. It is a common misconception that all skin growths are simply moles. Because certain early-stage skin cancers can mimic the appearance of benign growths, specialised dermatological examination, often using a dermatoscope to visualise underlying structures, is required to differentiate them. If a growth is symptomatic, such as causing bleeding, itching, or pain, or if it is evolving in size, shape, or colour, professional evaluation is the only way to ensure an accurate diagnosis and appropriate management.
What Are Common Classifications of Benign Skin Growth?
While all benign growths are non-cancerous, they are classified by the specific cell type from which they originate. Understanding the family of growth you have is essential for determining whether it can be safely monitored or if it requires removal.
Epidermal Growths
Connective Tissue and Fibrous Growths
Pigmented Growths
Vascular Growths
Cyst
Cysts are benign growths that can occur anywhere on the body. They usually appear as smooth, dome-shaped, soft to firm lumps underneath the surface of the skin. Some cysts may have an opening on the surface that looks like a comedo (blackhead). Various forms include epidermal (sebaceous) cysts, trichilemmal cysts, steatocystoma, milia cysts, etc.
Cysts contain fluid or semi-fluid material. Sometimes, this fluid can be expressed through the opening on the surface, and appear as a yellow to white, malodorous fluid.
Lipomas
Lipomas are benign growths composed of fat cells. These can occur anywhere on the body, be small or large in size, and be singular or multiple. Lipomas often feel soft and mobile, and lie deep underneath the surface of the skin.
Lipomas may be left alone if they do not cause any trouble. If treatment is desired, they can be removed by a small cut on the surface of the skin. This is a minor surgery performed under local anaesthesia in the clinic. If a lipoma starts to grow or becomes painful, one should see a doctor and have a biopsy to make sure the lump is not a liposarcoma, which is a rare but dangerous type of cancer.
Sebaceous Hyperplasia and Seborrhoeic Keratosis
Sebaceous hyperplasia is an enlargement of oil (sebaceous) glands on the face. They become more common with age. Sebaceous hyperplasia may be removed by a minor procedure under topical anaesthesia, such as electrocautery or laser.
Seborrhoeic keratoses are common, brown to black growths that are more commonly seen in people above the age of 40. They can range from a few millimetres to a few centimetres in size, and often have a rough or waxy surface. Large seborrhoeic keratoses may become irritated or inflamed when they are caught or rub against clothes. These growths can be treated by cryotherapy, or a minor surgery such as electrocautery or laser.
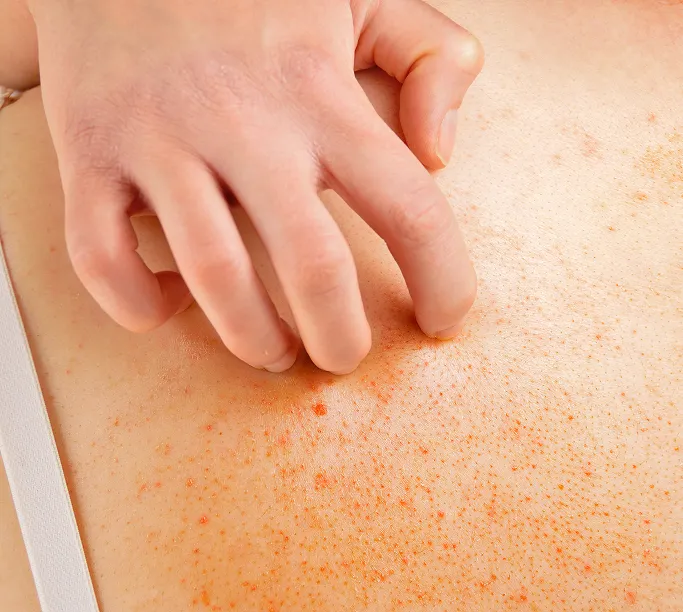
Common Symptoms of Benign Skin Growth to Look Out For
While benign skin growths are non-cancerous, they can sometimes cause irritation or be mistaken for more serious skin lesions. Monitoring your skin regularly helps you notice if a growth is behaving normally or if it requires a professional assessment. Here are the common signs to monitor:
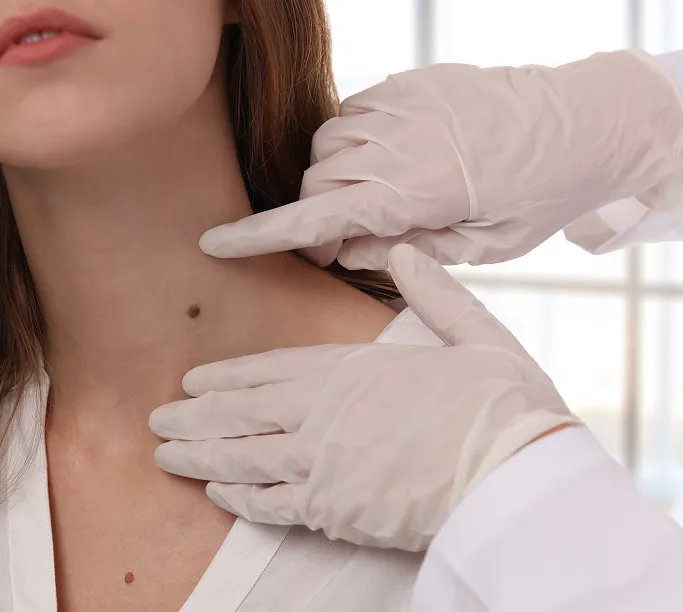
Changes in Appearance
Variations in Colour
Surface Texture and Integrity
Physical Sensations
Friction and Irritation
Sudden Onset
What Causes or Triggers Benign Skin Growths?
Benign skin growths arise from a wide range of biological miscommunications within different skin cell types. While each type of growth has a unique trigger, these are the most common contributors:
Cumulative Sun Exposure
Genetic Predisposition
Friction and Mechanical Stress
Ageing and Cellular Senescence
Viral Triggers
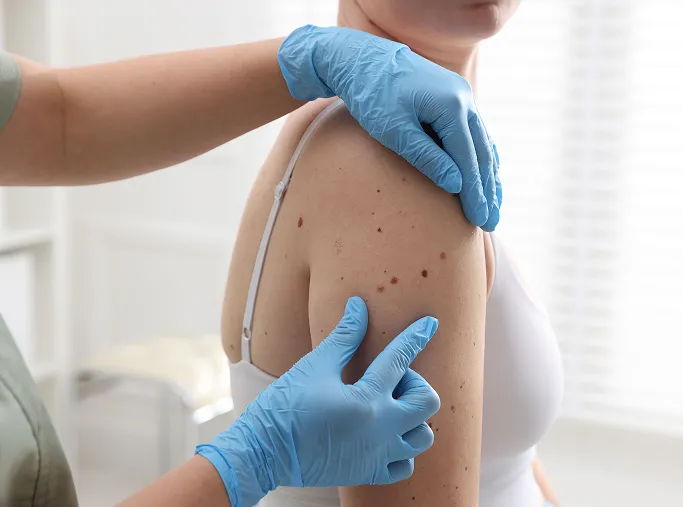
How Are Benign Skin Growths Diagnosed?
A dermatologist diagnoses a skin growth by evaluating its history, appearance, and clinical behaviour. While most are easily identified by sight, a comprehensive assessment ensures accuracy and rules out malignancy.
Clinical Examination and Dermoscopy
Medical History Review
Exclusion of Mimics
Diagnostic Biopsy
How Are Benign Skin Growths Treated at TSN Dermatology?
Our treatment approach focuses on safety, precision, and minimising scarring. We assess each growth individually to determine if removal is medically necessary or requested for cosmetic reasons.
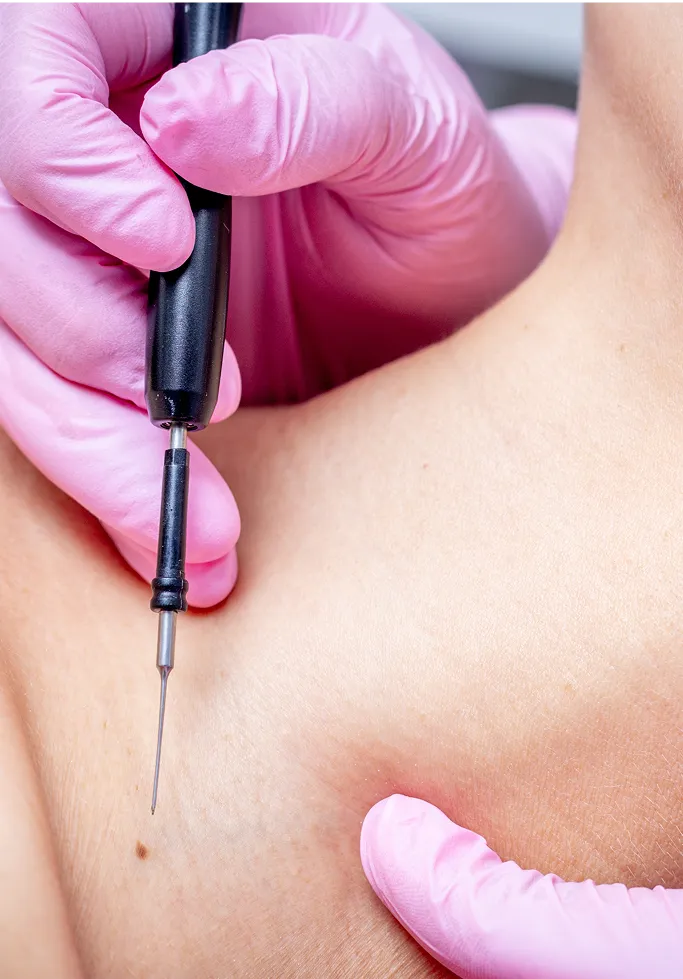
Individualised Treatment Approach
We begin by evaluating the growth's location, size, and type. If a lesion is in a high-friction area or shows signs of irritation, we prioritise removal. Our priority is always to achieve the best cosmetic outcome while ensuring the entire lesion is addressed to minimise the risk of recurrence.
Surgical and Procedural Removal
For growths that require complete removal, we offer several minimally invasive techniques:
Excision
A precise surgical removal for deeper lesions like cysts or larger dermatofibromas. We use fine-line suturing techniques to ensure the resulting scar is as subtle as possible.
Shave Removal
Often used for superficial growths like seborrheic keratoses or skin tags. This quick, efficient method involves shaving the lesion level with the skin surface under local anaesthesia.
Electrocautery
Using a specialised tool that delivers controlled heat to precisely burn away unwanted tissue, such as skin tags or certain small vascular growths, while simultaneously sealing blood vessels to minimise bleeding.
Cryotherapy
For superficial, waxy growths like seborrheic keratoses or viral warts, we utilise liquid nitrogen. By freezing the tissue, we induce a controlled reaction that causes the growth to gently detach and flake off over the following week, usually with minimal scarring, though temporary pigmentation changes may occur.
Laser and Light-Based Therapy
For vascular growths like cherry angiomas or certain pigmented lesions, we utilise medical-grade vascular lasers. These lasers target the haemoglobin in the blood vessels or the pigment in the lesion, effectively fading or removing the growth while minimising impact on surrounding healthy skin.
Post-Removal Care
Regardless of the removal method, we provide personalised aftercare instructions to support optimal healing. This may include:
Scar Prevention: Recommendations for silicone gels or specialised creams to ensure the skin heals smoothly.
Sun Protection: Essential for preventing hyperpigmentation at the site of removal.
Follow-up: A brief check-in to ensure the area has healed perfectly and that no further treatment is required.
Tips on Daily Care and Prevention of Benign Skin Growths
For individuals prone to benign skin growths—or for those who have recently had them professionally removed—daily care focuses on maintaining a healthy skin barrier, minimizing chronic irritation, and practicing excellent sun safety. While many benign growths are simply a matter of genetics or natural ageing, these habits can keep your skin comfortable and reduce the risk of future issues.
Sun Safety: Your First Line of Defence
-
Use Broad-Spectrum Sunscreen
UV radiation is a primary driver for many growths, including age spots and keratoses. Apply a high-SPF, broad-spectrum sunscreen daily to all exposed skin. -
Cover Up
In Singapore's intense tropical sun, wearing long sleeves, wide-brimmed hats, or UV-protective clothing provides superior protection compared to sunscreen alone, especially for areas like your arms and chest.
Minimise Friction and Mechanical Irritation
-
Choose Breathable Fabrics
Friction from tight clothing, collars, or bra straps can irritate existing skin tags or provoke new ones. Opt for soft, loose-fitting, natural fibers like cotton or bamboo to allow your skin to breathe and reduce rubbing. -
Avoid Removing it Yourself
Never try to cut, burn, tie off, or pick at skin growths, tags, or moles at home. This can lead to severe infection, excessive bleeding, permanent scarring, or the accidental removal of an undiagnosed lesion that required a biopsy.
Gentle Skin Hygiene
-
Use Mild Cleansers
Harsh scrubs or alcohol-based toners can strip your skin of natural oils and trigger inflammation in areas where growths are present. Stick to soap-free, pH-balanced cleansers. -
Keep Skin Dry
In humid climates, moisture trapped in skin folds (like the armpits or groin) can promote yeast or bacterial growth, which irritates skin tags and cysts. Gently pat these areas dry after showering.
Trigger Management
-
Manage Inflammation
If you are prone to inflammatory conditions like acne or folliculitis, manage them aggressively. Chronic inflammation often leads to reactive growths like dermatofibromas. -
Monitor Your Skin
Perform a monthly self-check. Use a mirror to look at areas you don't usually see, such as your back, scalp, and behind your ears. Get to know what is normal for your skin so you can quickly identify any new or changing lesions.
Post-Removal Aftercare
-
Follow Instructions
If you have recently had a growth removed, follow your dermatologist's wound care instructions strictly. -
Protect the Healing Site
Use silicone-based gels or healing ointments as recommended to minimise scarring. -
Strict Sun Protection
The new skin at a removal site is extremely vulnerable to sunlight. Keep it covered or protected with high-SPF sunscreen to prevent it from turning dark (hyperpigmentation).



When Should You See a Dermatologist for Benign Skin Growths?
While most benign growths are harmless, it is important to seek professional advice if you notice changes or if the growths become bothersome. Schedule a consultation if you experience any of the following:
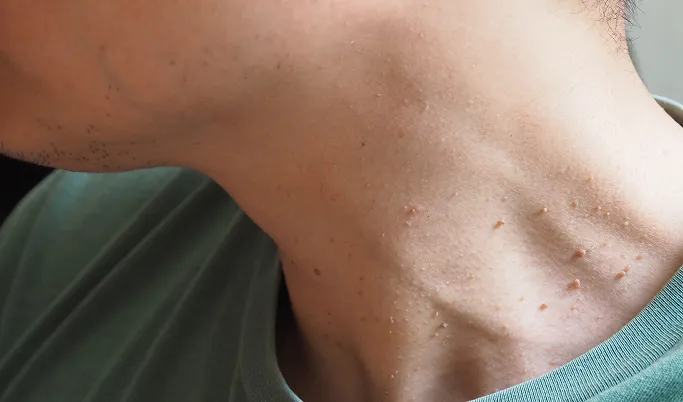
Rapid or Visible Changes
If a growth suddenly increases in size, thickness, or changes colour, it requires evaluation to rule out malignancy.
Persistent Symptoms
If a lesion becomes persistently itchy, tender, painful, or hot to the touch, this may indicate inflammation or secondary infection.
Bleeding or Non-Healing
Any growth that bleeds, crusts, or fails to heal after minor irritation should be checked immediately.
Cosmetic or Functional Distress
If a growth is in a highly visible area or a location where it repeatedly snags on clothing (such as skin tags on the neck or axilla), we can discuss safe removal.
Explosive New Growth
The sudden, widespread appearance of multiple new lesions across the body warrants a full skin check.
Uncertainty of Diagnosis
If you are unsure what a new bump or spot is, avoid the wait-and-see approach. A professional examination provides an accurate diagnosis and peace of mind, ensuring it is not a growth requiring specialised treatment.
FAQs About Benign Skin Growths
No. Benign skin growths are localised overgrowths of your own skin cells (such as pigment cells, connective tissue, or blood vessels). They cannot be spread through physical contact, sharing items, or social interaction. While some growths like warts are caused by a virus, they are not classified as tumors in the traditional sense and are distinct from other skin lesions.
These growths are often a reflection of your skin's genetics or natural ageing process rather than a disease. While a specific growth can be surgically or procedurally removed and will not come back in that exact spot, your skin may continue to develop new, similar growths over time as you age or continue to be exposed to environmental factors like the sun.
No. Most benign growths are strictly cosmetic. Removal is usually only recommended if the growth is symptomatic (bleeding, itching, or painful), located in an area of high friction, or if there is uncertainty about the diagnosis that requires a biopsy for confirmation.
This is largely down to your unique genetic blueprint and your skin's history. Factors like family history (genetics), cumulative sun exposure over your lifetime, and your skin type all dictate how many growths you develop. It is very common for these to appear or increase in number as you enter your 40s and beyond.
Most mature, benign skin growths (like seborrheic keratoses or dermatofibromas) are stable and will not disappear on their own. In rare cases, some growths may regress, but it is much more common for them to persist or slowly enlarge over time. If a growth disappears suddenly, it should be monitored, as this can occasionally indicate an inflammatory reaction.
Seek Proper Dermatologist Care for Benign Skin Growth
If you or your child have developed a skin growth, such as a mole, cyst, or skin tag, our specialists at TSN Dermatology Skin Specialist Clinic can assess the lesion, confirm whether it is benign, and recommend suitable treatment options. For more information or appointments, please contact us today.
Meet TheDoctors Behind Your Care

Dr Koh Hong Yi
Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in benign skin growth treatment, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh