Get In Touch
+65 64766821Book An Appointment

Dr Koh Hong Yi
Senior Consultant Dermatologist

Dr Tham Siew Nee
Senior Consultant Dermatologist
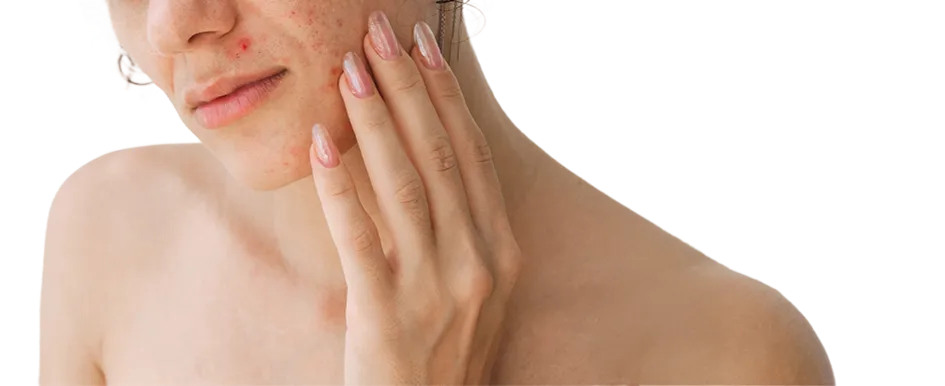
Acne vulgaris, commonly known as pimples, is a chronic inflammatory skin condition that affects both children and adults. While most prevalent in adolescents and teenagers, it is a common misconception that it only affects the young; it's not uncommon for some adults to continue to experience acne well into their 40s.
Acne typically affects the face, chest, shoulders, and back, where the concentration of sebaceous (oil glands) is highest. Although it is a common condition, treatment should be started early, as inflamed spots eventually give rise to unsightly scars that are more difficult and costly to manage.



What Is Acne?
Acne occurs when hair follicles (pores) become blocked by a combination of excess oil and sticky skin cells. This blockage prevents the natural release of sebum onto the skin surface, creating an environment where bacteria can thrive and trigger inflammation.
It is a complex medical condition involving hormonal changes, skin barrier dysfunction, and immune response, which is why professional dermatological care is essential for effective control and scar prevention.
What Are Common Types of Acne?
Acne is not a single, uniform condition. There are different types of acne depending on how the hair follicles and pores are affected. These lesions vary in appearance, severity, and level of inflammation. Common ones include:
Comedonal Acne
- The most common form, characterised by non-inflammatory lesions.
- Includes closed comedones (whiteheads) and open comedones (blackheads).
- Blackheads are not caused by dirt; they appear black because the trapped oil oxidises when exposed to air.
Papulopustular Acne
- Inflammatory acne that presents as small, red, tender bumps (papules) or pus-filled lesions (pustules).
- Can cause significant skin discomfort and often leaves behind post-inflammatory hyperpigmentation (dark spots).
- These are often the result of bacteria triggering a more significant immune response in the follicle.
Nodulocystic Acne
- A more severe form of acne involving deep, painful, and often large lesions beneath the skin's surface.
- Nodules are solid, tender bumps, while cysts are pus-filled, deeper, and carry a higher risk of permanent scarring.
- These types require prompt dermatological intervention to prevent long-term skin damage and address the underlying inflammatory process.
Hormonal Acne
- Often flares in adulthood, typically affecting the jawline and chin.
- Highly responsive to hormonal fluctuations, commonly seen in women before menstrual cycles or due to conditions like PCOS.
Acne Mechanica
- Caused by excess heat, friction, and pressure against the skin.
- Commonly seen in athletes or individuals wearing tight-fitting equipment, headbands, or backpacks that trap sweat against the skin.
Common Symptoms of Acne to Look Out For
Symptoms of acne can vary depending on the severity of the breakout and the individual's skin type. While some people may only experience occasional blemishes, others may deal with persistent, widespread inflammation. The following are the most common signs and features associated with acne.
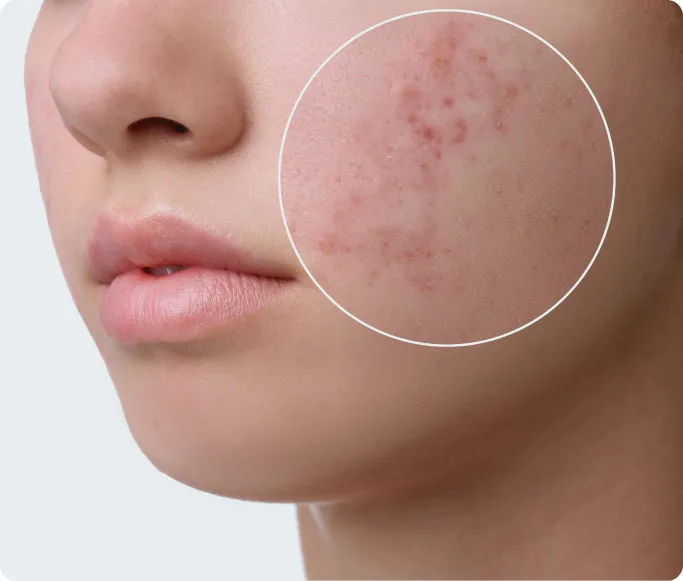
Whiteheads and Blackheads
Small, non-inflamed bumps that indicate blocked pores.
Papules and Pustules
Red, swollen bumps or white-headed pimples that may be tender to the touch.
Large, Painful Lumps (Nodules)
These are firm, deep-seated lesions that develop when the acne blockage is deep within the skin. They are often very painful and can feel like hard bumps beneath the surface.
Deep, Fluid-Filled Lesions (Cysts)
These are severe, inflammatory lesions that develop deep under the skin. They are often painful, carry the highest risk for permanent scarring, and may contain pus.
Oily Skin
Excessive sebum production is a common precursor to acne formation.
Post-Inflammatory Hyperpigmentation (PIH)
Dark or red marks left behind after a spot has healed, which can persist for months.
Scarring
Permanent indentations or textural changes resulting from severe or long-standing inflammatory acne.
What Causes or Triggers an Acne Flare-up?
Acne can be caused by various factors, which can include a combination of your skin's biology and your environment. It mainly happens when pores get clogged with excess oil, but various triggers can stir up these breakouts and make them harder to manage.
Hormonal Fluctuations
Dietary Factors
Friction and Pressure (Acne Mechanica)
Blockage of Pores
Improper Skincare Routine
Stress
Comedogenic Skincare
Humidity and Climate
Bacterial Growth
How Is Acne Diagnosed?
Diagnosing acne requires determining the specific type of lesion, underlying triggers, and the potential for long-term skin changes. To achieve an accurate diagnosis, your dermatologist will guide you through the following steps:
Clinical Examination
Medical History Review
Assessment of Hormonal Factors
Exclusion of Mimicking Conditions
Evaluation of Lifestyle and Product Use
Diagnostic Testing (If Required)
How is Acne Treated at TSN Dermatology?
Effective acne management focuses on controlling active breakouts, preventing new lesions from forming, and reducing the risk of long-term skin changes such as pigmentation and scarring. Early treatment is important, as inflamed acne can damage deeper layers of the skin and lead to scars that are more difficult and costly to treat.
At TSN Dermatology, treatment is tailored according to each patient's skin condition and contributing factors. A range of medical therapies may be recommended to address different types and severities of acne.

Individualised Treatment
A tailored acne treatment allows the dermatologist to address underlying causes of acne, optimise treatment outcomes, and reduce the likelihood of pigmentation or scarring. Treatment decisions are guided by factors such as:
The type and severity of acne (e.g., comedonal, inflammatory, or cystic)
The location of the breakouts (e.g., face, back, or jawline)
Presence of post-inflammatory hyperpigmentation or scarring
Age and lifestyle factors, including potential hormonal triggers
The impact on the patient's self-esteem and daily life
Topical Treatments
Topical therapy is the cornerstone of acne management for many patients. We use targeted treatments to clear existing lesions and prevent new ones from forming:
Mild Acne: Typically managed with topical agents such as retinoids (vitamin A derivatives), antibiotics, benzoyl peroxide, or azelaic acid to clear pores and reduce bacteria.
Moderate to Severe Acne: May require systemic support, including oral antibiotics, oral retinoids (such as isotretinoin), or hormonal therapy to target the root causes from within.
Oral Medications
For moderate to severe or scarring acne, we may prescribe oral antibiotics, hormonal therapy (such as oral contraceptives or spironolactone), or oral isotretinoin to address deeper, treatment-resistant acne.
Procedural Treatments
Beyond medications, we provide clinical procedures to help manage acne and improve skin texture:
Medical-Grade Extractions: Safely removes persistent blackheads and whiteheads to speed up clearance and prevent further inflammation.
Chemical Peels: Customised professional-grade peels can help unclog pores, reduce oil production, and smooth out skin texture.
Laser and Light-Based Therapies: Certain light treatments can help reduce bacterial load and minimize the redness associated with inflammatory lesions, providing a non-drug alternative or adjunct for some patients.
Tips on Daily Acne Care and Flare Prevention
Gentle Cleansing and Bathing
Hands Off
Non-Comedogenic Products
Sun Protection




When Should You See a Dermatologist for Acne?
While many people attempt to manage breakouts with over-the-counter (OTC) products, acne sometimes requires proper medical intervention. Consider seeing a dermatologist if you notice any of the following:
Lack of Progress
If you have consistently used acne-fighting ingredients like benzoyl peroxide, salicylic acid, or topical retinoids for 8 to 12 weeks without noticeable improvement, your skin likely requires prescription-strength intervention.
Painful or Deep Lesions
Seek help if your breakouts are deep, throbbing, or physically tender to the touch. These are often signs of nodular or cystic acne, which carry the highest risk of long-term tissue damage.
Widespread Coverage
If your acne is extensive, affecting large areas of your face, back, or chest, it is often too systemic to be managed with basic OTC products.
Signs of Permanent Damage
If you notice your skin is leaving behind stubborn dark marks (post-inflammatory hyperpigmentation) or beginning to develop permanent pitted or raised scars, professional treatment is necessary to halt the process.
FAQs About Acne
No, acne is not contagious. You cannot catch it from someone else or spread it through physical contact, sharing items, or social interaction. Acne is a medical condition driven by internal factors—such as hormones, oil production, and inflammation within your own hair follicles—not by an infection that can be passed between people.
Acne can be effectively treated when it is viewed as a manageable medical condition rather than a temporary phase you just have to outgrow. While there isn't a single instant cure that makes acne disappear forever, the vast majority of our patients reach long-term, clear skin through a consistent, tailored care plan.
While many people see a significant improvement in their acne after their teenage years, adult-onset acne is increasingly common. For some, hormonal or environmental factors mean that breakouts can persist or first appear well into adulthood, necessitating ongoing management.
Yes. Untreated inflammatory acne—particularly deep nodules and cysts—can cause permanent scarring or long-lasting dark spots (post-inflammatory hyperpigmentation). Seeking early treatment is the most effective way to prevent these lasting skin changes.
Seek Proper Dermatologist Care for Acne
If you or your child are experiencing persistent or worsening acne, a consultation with our specialists at TSN Dermatology Skin Specialist Clinic can help clarify the diagnosis and establish an effective, personalised treatment plan focused on long-term skin health and quality of life. For more information or appointments, please contact us today.
Meet TheDoctors Behind Your Care

Dr Koh Hong Yi
Senior Consultant Dermatologist
Bachelor of Medicine, Bachelor of Surgery (MBBS)
Member of the Royal College of Physicians (United Kingdom)
Master of Medicine (Internal Medicine)
Fellow of the Academy of Medicine, Singapore (Dermatology)
Dr Koh Hong Yi is a Ministry of Health-accredited dermatologist with over 20 years of experience in medical, surgical and aesthetic dermatology.
He trained in Singapore and the UK, and is particularly interested in acne treatment, Mohs micrographic surgery, dermatologic surgery, skin cancer care, and inflammatory skin diseases.
Prior to private practice, he founded the Mohs Surgery Service at Singapore General Hospital and served as consultant dermatologist and Adjunct Assistant Professor with Duke-NUS Medical School, contributing to clinical research and education.
About Dr Koh